Last Updated on September 12, 2019
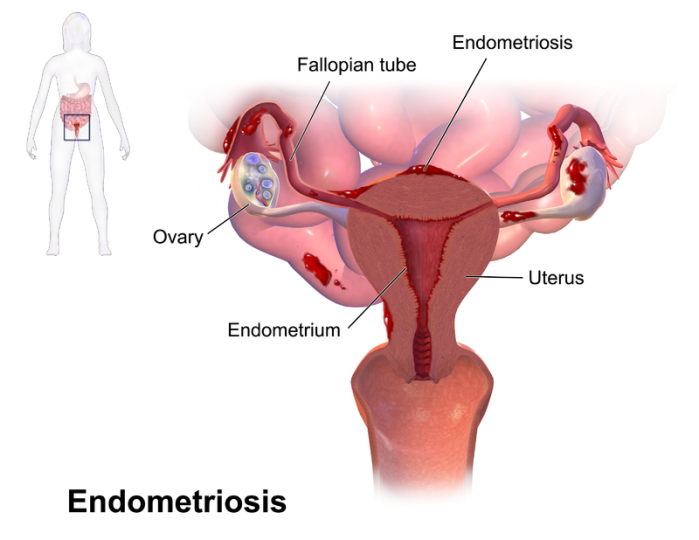
Endometriosis is a disorder in which tissue that normally lines the inside of the uterus (the endometrium) grows outside the uterus. Endometriosis most commonly involves the ovaries, fallopian tubes and the tissue lining the pelvis. Rarely, it may spread beyond pelvic organs.
This abnormally placed endometrial tissue continues to act as the normal endometrium. Due to cyclic changes in hormones which occur normally in women, this abnormal endometrium also undergoes thickening, tissue break down and bleeding with each menstrual cycle. As this displaced tissue and blood has no way to exit the body, it becomes trapped within the organ. This can irritate the surrounding tissue resulting in the development of scars and adhesions which result in organs sticking to each other.
The exact incidence in the general population is unknown, as the definitive diagnosis requires biopsy or visualization of the endometriotic implants at laparoscopy or laparotomy.
It affects approximately 6-10% of women in the general population.
It usually affects reproductive-aged women. Almost one-fourth to one-half of women presenting with infertility suffer from endometriosis. Patients presenting with chronic pelvic pain and severe dysmenorrhea show a much higher incidence of endometriosis.
Signs and Symptoms
Painful periods (dysmenorrhea)
The main symptom of endometriosis is pelvic, lower back or abdominal pain, often associated with the menstrual period. Although some degree of discomfort and cramping during menses is common in women of all ages, patients with endometriosis experience far greater pain than usual. The pain is progressive in nature ie, it tends to increase over time. Pain may begin a few days before the start of periods and continue during and for several days after the end of menstruation.
Infertility
It is the second most common symptom. Endometriosis is first diagnosed in some women who are seeking treatment for infertility.
These patients usually have inflammation and adhesions present in the ovary and pelvic area which interferes with ovulation, fertilization, implantation and various aspects of conception. Adhesions may lead to distorted fallopian tubes and ovaries. This places the patients at a greater risk for ectopic pregnancies, which occurs when the fertilized egg gets implanted in the tube and not in the uterus. It has also been suggested that inflammation produces certain chemicals which may interfere with egg quality and release.
Chronic pelvic pain
Many patients experience a chronic nagging kind of the pain in the pelvic area, lower back or abdomen at all times.
Pain during intercourse (dyspareunia)
Pain during or after sex is common with endometriosis.
Pain during bowel movements or urination
Increased frequency of urine, urinary urgency and pain during voiding or passage of stools may be present in these patients. These symptoms occur more commonly during menses.
Excessive bleeding
Both heavy periods (menorrhagia) or bleeding between periods (menometrorrhagia) are associated with endometriosis.
Other non-specific symptoms
These may include fatigue, diarrhea, constipation, bloating or nausea, especially during menstrual periods.
Causes
The exact cause of endometriosis is not known. However several possible explanations have been put forward. It is believed that the interplay between several factors is responsible for causing endometriosis.
Retrograde menstruation (implantation theory or transplantation theory)
It is the most widely accepted theory for the formation of endometriosis. According to it, during menstruation, some of the endometrial cells and debris flow backwards through the fallopian tubes and into the pelvic cavity instead of flowing out of the body through the vagina. These displaced endometrial cells invade the pelvic walls and organs and grow as endometriotic foci.
Transformation of peritoneal cells (induction theory)
Under the influence of hormones, inflammation or immune factors, the peritoneal cells which line the inner side of the abdomen, transform (undergo metaplasia) into endometrial cells.
Transformation of stem cells (Mullerian theory)
During embryonic development, some of the cells from the female reproductive tract or Mullerian tract become dislocated and act like stem cells. These cells transform into endometrial cells. This theory is able to explain endometriosis found in organs distant from the pelvis such as the brain or lungs.
Surgical scar implantation
Endometrial cells may get attached at the site of surgical incision following any laparoscopic or laparotomy procedure including hysterectomy or Cesarean-section.
Transportation of endometrial cells
Endometrial cells may be transported to different parts of the body through blood vessels or lymphatic channels.
Immune system disorder.
An altered immune response in some patients does not allow the body to recognize and destroy abnormal endometrial tissue.
Environmental toxins
Certain chemicals and toxins present in the environment have been linked to endometriosis. Role of dioxin is being investigated although no definite link has so far been established.
Genetics
Genetic predisposition is thought to play a role. Low progesterone levels leading to a hormone imbalance may be hereditary. There is a higher risk of developing endometriosis in women having an affected first-degree relative.
Locations
Endometriosis can occur anywhere in the body. Common sites include:
• Ovaries (most common site)
• The peritoneum between the back of the uterus and the rectum (Pouch of Douglas)
• Fallopian tubes
• The ligaments connecting the uterus to the abdominal wall
• The outer surface of the uterus
• Sites of a surgical abdominal incision (scar endometriosis)
• Less common sites include vagina, cervix, vulva, bowel, bladder, rectum, diaphragm
• Very rarely, it is found in the arms, legs, nose, lungs, brain or skin. If a woman gives a history of bleeding from the nose or any other external body part which synchronizes with the menstrual period, then endometriosis should be strongly suspected.
Staging of Endometriosis
(Revised classification of the American Society of Reproductive Medicine 1997).
Endometriosis is divided in 4 categories depending upon the location, extent, and depth of lesions and adhesions present in pelvic organs.
Staging does not always correlate with signs and symptoms. A person with Stage I endometriosis may experience severe pain, while a person with Stage IV disease may have no symptoms.
Staging assesses physical disease only.
Stage I (Minimal)
There are small and superficial endometrial implants on the ovary. No adhesions are present.
Stage II (Mild)
In addition, some deep lesions are present in the cul-de-sac (the space between the uterus and rectum).
Stage III (Moderate)
Deep implants are present in the ovary along with adhesions. Endometriomas or chocolate cysts may also be present.
Stage IV (Severe)
Deep implants are present on the pelvic lining and ovaries along with extensive adhesions. There may also be lesions on the fallopian tubes and bowels.
Relation between endometriosis and cancer
Endometriosis is not a cancerous condition per se. However, the presence of endometriosis increases the risk of certain types of epithelial ovarian cancers. There is also a slightly increased risk of developing non-Hodgkin’s lymphoma and breast cancer.
Diagnosis of Endometriosis
Clinical Presentation
Typical symptom of severe pain, especially in the pelvic area and related to menstruation is a very important clue for suspecting endometriosis.
Pelvic examination is done to palpate areas in the pelvis for any abnormalities. Any lumps, cysts or scars in the reproductive organs or pelvic area are looked for.
Ultrasound
This can be done either through the abdominal wall or through the vagina (transvaginal ultrasound). It can help to identify endometriotic cysts (called endometriomas).
Laparoscopy
It is a surgical procedure in which a slender viewing instrument (laparoscope) is inserted into the abdomen to visualize the pelvic and abdominal organs. It is carried out under general or spinal anesthesia.
This enables the surgeon to visualize any lesion present inside the abdominal cavity, its exact location along with the extent and size. Endometriotic lesions can appear dark blue, black, red, white or yellow in color.
Larger lesions may be seen within the ovaries. These are called endometriomas or chocolate cysts (named so because they contain chocolate-like thick brownish fluid which is mainly old blood). A sample of tissue (biopsy) is also taken from the suspected lesion to examine it microscopically.
Besides helping in diagnosis, this procedure also serves as a surgical treatment of endometriosis at the same time.
At times, no lesions are found in women presenting with typical symptoms. In such cases, other diagnoses including adenomyosis, pelvic adhesions, pelvic inflammatory disease, congenital anomalies of the reproductive tract, and ovarian or tubal masses which show similar signs and symptoms need to be considered.
Histopathology (Biopsy)
It remains the gold standard for diagnosing endometriosis. While signs or symptoms and even laparoscopic evaluation of the lesions can only suggest the diagnosis, confirmation is obtained only through histopathological examination of the biopsy obtained during surgery.
Microscopic evaluation of the lesions shows endometrial glands, endometrial stroma, and hemosiderin-laden macrophages. Two out of these three features should be present to diagnose endometriosis.
Sometimes, in old cases, due to repeated episodes of hemorrhage, endometrial glands and stroma are not seen. Only blood, pseudoxanthoma cells, and hemosiderin-laden macrophages are seen along with areas of fibrosis indicative of recent and old hemorrhage (burnt out endometriosis). In such cases, only a presumptive diagnosis of endometriosis can be made.
Immunohistochemistry is sometimes used as an adjunct to biopsy. CD 10 [immunohistochemical marker] stains the endometrial stromal cells and is used to confirm the presence of tiny endometrial tissue that is missed on routine microscopy.
Biochemical marker
CA-125 is moderately elevated in endometriosis. Very high values are usually associated with ovarian cancers.
Medical Treatment of Endometriosis
Painkillers
Nonsteroidal anti-inflammatory drugs (NSAIDs) or opioids are commonly used as a first-line treatment to help relieve pelvic pain and menstrual cramping. These drugs provide only symptomatic relief but have no effect on the progression of endometriosis.
As the diagnosis of endometriosis can only be confirmed with a biopsy, most of the patients suspected of having endometriosis are treated for pain initially without a definite diagnosis being established. If they are effective in giving symptomatic relief from pain, no other diagnostic procedure or treatments is usually carried out. If they do not provide adequate relief, further evaluation and treatment options are considered.
Hormone therapy
The hormonal changes that occur normally during the menstrual cycle cause endometrial implants to grow to break down and bleed. Hormone medication can slow the growth of these implants and also prevent the formation of new implants.
Patients who present with infertility and want to get pregnant are not given hormonal therapy since it suppresses ovulation and delays the pregnancy.
Gonadotropin-releasing hormone (Gn-RH) analogs.
These drugs block the production of ovarian-stimulating hormones from the pituitary gland, thereby, decreasing estrogen levels and preventing menstruation. This causes endometrial tissue to shrink. Since these drugs create an artificial menopause, taking a low dose of estrogen or progestin along with Gn-RH analogs can eliminate the menopausal side effects, such as hot flashes, fatigue, mood alterations, vaginal dryness, bone loss, etc. This menopause-like state is reversible and the patient can get pregnant once the medication is stopped.
Oral contraceptive pills
Oral contraceptive pills (combination of estrogen and progesterone) help control the hormones responsible for the buildup of endometrial tissue each month. These pills result in short and reduced menstrual flow. Continuous cycle regimens which means a continuous use of the pill by skipping the hormonally inert part of the cycle does not allow menstruation to occur. It is useful in reducing the pain of mild to moderate endometriosis.
Progestin therapy
Progesterone counteracts the effect of estrogen and thus inhibits the growth of the endometrial implants. It also leads to a cessation of menstrual periods. It is more potent than oral contraceptive pills and is recommended for women in whom oral contraceptive pills are ineffective or contraindicated. Since the absence of menstruation induced by high doses of progestins can last for several months even after stopping the therapy, these drugs should be avoided in women who are planning pregnancy in near future.
Danazol
This drug produces an androgen (male hormone) like effect. It lowers the estrogen level and interferes with ovulation. It causes shrinkage of endometriosis implants and pain relief in the majority of the women. However, it is not a preferred drug because it can cause side effects like hirsutism and voice changes and can be harmful to the baby if the patient gets pregnant while taking this medication.
Aromatase inhibitors
These are drugs that only inhibit estrogen production within the ovary and adipose tissue but also locally within the endometriosis implants. Examples include anastrozole and letrozole. These drugs have been introduced recently and studies and experiments are still being carried out to determine their efficacy. So far they have shown positive results in pain control.
Surgical Treatment of Endometriosis
Conservative surgery
Conservative surgery is carried out for women who want to get pregnant. The main aim of this surgery is to remove or destroy endometrial growths and lyse peritubal and periovarian adhesions without damaging the reproductive organs.
The laparoscopic approach is the method of choice for treating endometriosis conservatively. Ovarian endometriomas can be either drained or removed by laparoscopy or open laparotomy.
Laparoscopic ablation (or destruction) can be performed with laser or electrodiathermy.
About one-fourth to one-half of the patients undergoing conservative surgery experience recurrence over 2–5 years.
Semiconservative surgery
This involves removal of uterus and cervix (hysterectomy) and destruction or removal of endometrial implants. Ovaries are preserved in these patients. It is carried out in women who have completed their families but are too young to undergo surgical menopause.
Chances of recurrence are higher in these patients compared to those whose ovaries are also removed.
Radical surgery
This involves removal of uterus and cervix along with both the tubes and ovaries. Any visible endometrial implants are also resected. Since the ovaries are removed, estrogen production is stopped and the stimulus to remaining endometriosis implants is removed. It is a last resort treatment for women who have completed their families.
Long-term complications include an increased risk of heart and blood vessel (cardiovascular) diseases and certain metabolic conditions.
Nerve transaction procedures
In women having extreme pain, nerves which supply the uterus may be cut to produce relief from severe pain. In presacral neurectomy, the nerves at the level of the third sacral vertebra are cut. In laparoscopic uterine nerve ablation (LUNA), the uterine nerve fibers that exit the uterus through the uterosacral ligament are cut.
Both these procedures have a high incidence of complications including vascular injury, constipation, uterine prolapse, etc and are very rarely performed. Few recent studies have shown no beneficial effects from these procedures.
Management of Infertility related to Endometriosis
Assisted reproductive technologies, such as in vitro fertilization (IVF), can be carried out to tackle infertility associated with endometriosis.
How to prevent Endometriosis
There is no definite way to totally prevent endometriosis. Risk can, however, be reduced by lowering the body estrogen’s levels. The following factors have been found to reduce the chances of getting endometriosis.
- Regular exercise
- Eating a healthy and whole-food rich diet
- Reducing the amount of alcohol intake
- Avoiding large amounts of caffeinated drinks
- Reducing exposure to xenoestrogens
- Xenoestrogens are chemicals which produce an estrogen-like effect on the body but their chemical structure is different from endogenous estrogen.
- Common sources of xenoestrogens include commercially raised meat and dairy products, items with insecticide or pesticide residue, tap water, artificial food additives, etc.
- Examples are atrazine, bisphenol A (BPA), dioxin, polybrominated biphenyls
