Last Updated on November 20, 2017
Central pontine myelinolysis is a concentrated, frequently symmetric, noninflammatory demyelination within the central Basilar part of pons. In at least 10% of patients with central pontine myelinolysis, demyelination also occurs in extrapontine regions, including the mid brain, thalamus, basal nuclei, and cerebellum.
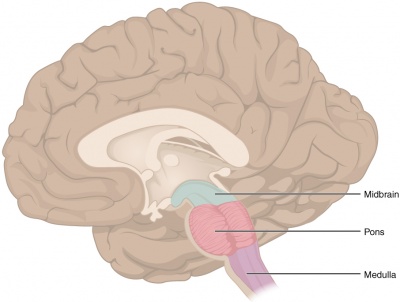
The exact mechanism that strips the myelin sheath is unknown though the proposed mechanism says cellular edema, is caused by fluctuating osmotic forces, results in compression of fiber tracts and induces demyelination.
Central pontine myelinolysis occurs as a complication of severe and prolonged hyponatremia, particularly when corrected too rapidly.
The exact incidence of central pontine myelinolysis is unknown.
Causes
Conditions predisposing patients to central pontine myelinolysis include alcoholism, liver disease, malnutrition, and hyponatremia.
Risk factors for central pontine myelinolysis in the hyponatremic patient include the following:
- Serum sodium of less than 120 mEq/L for more than 48 hours
- Aggressive IV fluid therapy with hypertonic saline solutions
- Development of hypernatremia during treatment
Many patients who have hyponatremia that is corrected rapidly do not develop central pontine myelinolysis. Thus, other less obvious risk factors probably exist. Central pontine myelinolysis reportedly occurs occasionally in patients who are treated for hypernatremia.
Central pontine myelinolysis may complicate liver transplantation surgery.
Burn patients with a prolonged period of serum hyperosmolality are prone to developing central pontine myelinolysis. Central pontine myelinolysis also has occurred concurrently with Wilson disease and neoplasia.
Clinical Presentation
There is a history of severe hyponatremia and its correction. Serum sodium becomes normal the next day and the patient’s mental status improves.
But this is followed by neurologic deterioration 48-72 hours later.
Examination reveals confusion, horizontal gaze paralysis, pseudobulbar palsy [head and neck weakness, dysphagia, and dysarthria.] and spastic quadriplegia [Increased limb tone, limb weakness, hyperactive reflexes, and Babinski sign]
Brain MRI reveals intense symmetric demyelination in the brain stem pons. [10, 11]
Delirium is extremely common.
Sensory abnormalities in sensory modalities usually are not observed.
A large basis pontis lesion may cause a locked-in syndrome, which includes paralysis of lower cranial nerves and limb musculature. Vertical eye movements, blinking, breathing, and alertness may remain intact in these patients.
Diagnostic Tests
IF the cause and diagnosis is certain, the CSF examination is not required. CSF studies may demonstrate increased opening pressure, elevated protein, or mononuclear pleocytosis.
MRI is the imaging of choice and T2-weighted MRI images demonstrate hyperintense or bright areas where demyelination has occurred but in some cases the image may not show the disturbances
Electroencephalography in central pontine myelinolysis may demonstrate diffuse bihemispheric slowing. Brainstem-evoked potentials may reveal abnormalities when neuroimaging is unrevealing.
Treatment
Treatment is supportive only. It is best to prevent the risk by correcting hyponatremia at a slower rate.
Patients with alcoholism should receive vitamin supplementation.
Once medically stable, rehabiliatation should be started.
Maximum recovery from central pontine myelinolysis may require several months.
Death is common.
Chronic neurologic deficits range from locked-in syndrome to spastic quadriparesis. Patients with extrapontine lesions may exhibit tremor and ataxia.
Following complications may be seen
- Ventilator dependency
- Aspiration pneumonia
- Venous thrombosis
- Pulmonary embolism
- Contractures
- Muscle wasting
- Decubitus ulcers
- Urinary tract infections
- Depression
References
- Singh TD, Fugate JE, Rabinstein AA. Central pontine and extrapontine myelinolysis: a systematic review. Eur J Neurol. 2014 Dec. 21 (12):1443-50.
- Laureno R, Karp BI. Myelinolysis after correction of hyponatremia. Ann Intern Med. 1997 Jan 1. 126(1):57-62.
- Graff-Radford J, Fugate JE, Kaufmann TJ, Mandrekar JN, Rabinstein AA. Clinical and radiologic correlations of central pontine myelinolysis syndrome. Mayo Clin Proc. 2011 Nov. 86(11):1063-7.
