Last Updated on October 29, 2023
Tinea is a fungal skin infection. It is commonly known as ringworm but the spectrum of tinea is far wider. Most conditions identified as tinea are members of the imperfect fungi that make up the dermatophytes. However, conditions such as Tinea nigra and Tinea versicolor are not caused by dermatophytes.
Dermatophytes live on keratinous structures and thus, can infect the epidermis (stratum corneum only) as in the hair and the nails. The dermatophytes responsible for human infections belong to three generations.
- Microsporum
- Trichophyton
- Epidermophyton.
Some of these dermatophytes live only on the human body and are thus, called anthropophilic. Others infect mainly some pet animals such as dogs, cats, horses or cattle and are called zoophilic.
A few dermatophytes thrive in the soil and are called geophilic.
Thus a man can get infected from other infected individuals or animals or from the soil.
The infectivity of these dermatophytes is very low and therefore, prolonged contact is necessary before an individual can get infected.
People on corticosteroids or other immunosuppressive drugs are more prone to infection by these agents. These patients may develop widespread dermatophytosis that keeps recurring.
These infections are more in hot and humid climates. Synthetic clothes during summer may also increase the susceptibility.
The clinical picture of dermatophytosis varies depending upon the site of infection.
Clinical Presentation
Tinea cruris
When similar well-defined lesions are situated in the groins, the condition is called tinea cruris. It occurs only in adults especially males and not in children. Wearing clothes made of synthetic materials such as terylene and nylon, which tend to accumulate heat and humidity in the skin makes the condition worse.
Tinea pedis and tinea manus
Fungus infection of the soles and palms usually manifests as circumscribed areas of scaling and fissures. Sometimes, papulo-vesicles and even pustules may also be superimposed on this area. Itching is always severe in these cases. In addition, the skin usually shows some hyperpigmentation.
More commonly, however, the interdigital space between the adjoining toes or fingers shows maceration and erythema with or without papulo-vesicular lesions. This is called tinea interdigitale and is often asymptomatic. Many times, the patient is not even aware of this silent infection which may be acting as a source of infection for other areas.
Tinea pedis and tinea manus also occur only in adults. Tinea interdigitale is particularly common in persons who have flat apposing surfaces of the adjoining toes and also those who wear boots and nylon socks in summer months. It is thus called a disease of civilization. Rarely, tinea pedis and tinea manus may manifest as recurrent eruptions of severely itchy vesicular lesions on both the palms or soles.
Tinea Unguium
Fungus infection of the nails is called tinea unguium. It generally starts with the involvement of a single nail, though other nails may also get infected in due course. Involvement of all the 20 nails of the fingers and toes can occur but is rare. The infection can primarily involve the nail bed when it starts from the distal edge and progresses proximally.
It leads to the deposition of a powdery material under the nail plate which gets lifted up. The nail plate also may get thickened and discolored. When the nail plate is primarily involved, the nail plate becomes brittle and disintegrates. This also starts at the distal edge and leads to an appearance as if the nail plate has been eaten away.
The remaining part of the nail plate may become thickened, dull, and discolored. There is, as a rule, no itching unless the adjoining skin is also involved. Invasion of the nail plate from the surface may produce dull-white areas on the nail plate called leuconychia trichophytica.
Tinea Capitis
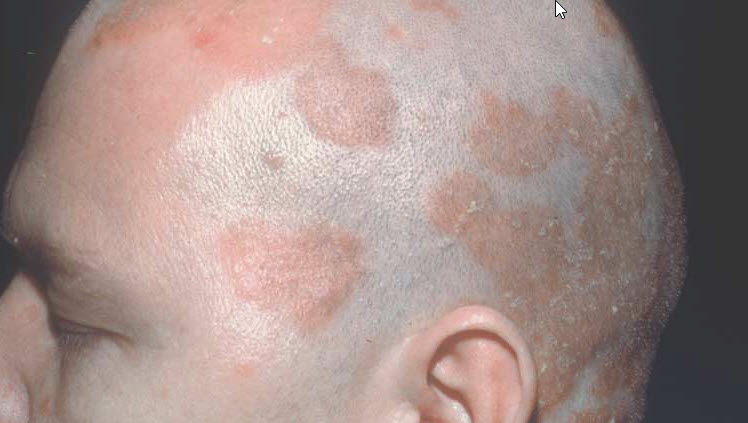
This term is used when the infection primarily involves the scalp hair. It occurs mainly in children and is very rare in adults because it is believed that the sebaceous secretion in adults protects the skin from fungus infection.
Mustard oil has a weak anti-fungal effect and thus local applications of mustard oil are expected to protect from fungal infection. Presentation of the disease varies.
The patient may have scaly grey single or multiple patches consisting of an itchy area of alopecia. The skin has a dry scaly appearance with a very mild degree of erythema. The hair in the region is sparse, dry, lusterless, brittle, and broken at varying lengths.
Another variety also has a dry scaly appearance, but the itching and scaling are much less, and the hairs are broken at the level of the skin surface producing a picture of black dots in an area of alopecia. This type is commonly caused by Trichophyton violaceum.
Kerion is the term used when the fungus produces a boggy swelling on the scalp because of the increased inflammatory response initiated by the fungus. There is usually no pus, and often it is not possible to demonstrate the causative fungus in the stumps of the broken hairs. This type of tinea capitis is commonly caused by Trichophyton mentagrophytes.
Favus is the lesion that characteristically consists of 4-10 mm size cup-shaped yellowish crusts called scutula with a mousy odor, present in localized patches on the scalp. Removal of the crusts leaves behind superficial erosions.
Tinea barbae
When the fungus involves hairs in the beard region it is called tinea barbae. The lesions consist of one or more localized boggy swellings resembling kerions. It occurs only in adult males.
The infected hairs can be easily pulled out without causing much pain.
Tinea corporis
Primary infection of the surface of the skin of the trunk, face, and extremities is called tinea corporis and manifests in the form of severely itchy, circular, or irregular lesions which have well defined active borders made up of papulo-vesicles, while the central parts of the lesions show hyperpigmentation, erythema, and slight scaling.
These lesions are commonly known as ringworms.
The abdomen is quite commonly involved especially in the belt region. Most cases of tinea corporis are caused by Trichophyton rubrum and the fungus remains confined to the stratum corneum only. The inflammation in the skin is produced by the metabolites of the fungus which permeate through the skin. The fungus does not penetrate into the living cells of the epidermis.
If one applies corticosteroid ointments, the classical clinical features of tinea corporis may be masked. Such cases are labeled as tinea incognito. This should be suspected if the lesions tend to be patchy but do not have well-demarcated margins.
Sometimes, it is possible to demonstrate the fungus as well, but a therapeutic response to anti-fungal treatment should suggest the diagnosis.
Tinea is known by the region it affects like Tinea capitis in the head, Tinea pedis in the foot, etc.
Diagnosis of Tinea Infections
The diagnosis in each case can be confirmed by demonstrating the presence of the fungus (hyphae) in scrapings from the skin, nails, or hair as the case may be. In the case of tinea capitis and tinea barbae, one should pull out the infected hairs which are dull, lusterless, and broken.
In tinea corporis, the scrapings should be taken from just inside the active border of the lesion. In tinea cruris and tinea interdigitale, it is preferable to take the macerated tissues.
In tinea unguium, one should take either the clipping of the nail plate or collect the powdery material from beneath the nail plate. In case the patient has blisters, one should examine the roof of the blister and not the blister fluid because the fungus remains confined to the stratum corneum only.
The material should be mounted on a microscopic slide in a drop of ten percent KOH. KOH helps to dissolve the keratin cells and liberate the fungus and thus any other strong alkali may also be used if KOH is not available. It generally takes 30 minutes for the KOH to dissolve the keratin, though, in winter, it may take longer. Nails may take two to three hours or an overnight incubation may also be necessary.
The presence of hyphae and spores establishes the diagnosis. Scrapings can be negative if the patient has already used anti-fungal agents or if the lesion is too inflammatory as in a kerion. The causative fungus can also be cultured on Sabourud’s medium where the fungal colonies appear in approximately two weeks’ time.
Treatment
Following is the generalized approach to treatment and can be individualized depending on the patient.
Local Measures
The patient should be encouraged to clean the area with soap and water during bathing. Cotton clothes are preferable as wearing material. Patients having lesions on the feet should be encouraged to wear open footwear such as chappals or sandals instead of socks and boots.
A large number of anti-fungal agents are available for local application which are almost equally effective.
Whitfield’s ointment, containing three percent salicylic acid and six percent benzoic acid in petrolatum base is a traditional remedy. It should be massaged into the lesions once or twice a day.
Benzoic acid is a moderately strong anti-fungal agent, while salicylic acid acts as a keratolytic agent and helps in exposing the fungus to the action of benzoic acid.
Castellani’s paint is a deep red colored liquid which is also very effective when applied once or twice a day. It is especially recommended for tinea interdigitale or when there are vesicular lesions on the palms and soles.
The paint can be prepared by adding 10 ml of a 5% aqueous solution of basic fuchsin to 4 ml of a 5% aqueous solution of carbolic acid. The mixture should be allowed to stand for one hour and then filtered. To the filtrate should be added 10 gm of boric acid and kept for three hours. This should be followed by the addition of 2 gm of resorcin and 10 ml of acetone and the total volume should be made to 100 ml with water. After one hour, Castellani’s paint is ready for use.
Application of 5% aqueous silver nitrate followed by tincture iodine results in the formation of silver iodide on the skin which acts as an anti-fungal agent. Such applications are to be applied once a day as repeated applications of silver nitrate can lead to significant systemic absorption of silver.
Currently, however, the commercially available proprietary anti-fungal creams or ointments are preferred. These medicines contain derivatives of quinoline, undecylenic acid, tolnaftate, miconazole, econazole, clotrimazole, or ciclopirox.
Local applications of the anti-fungal agents twice a day generally lead to improvement of the clinical condition within two or three days.
If there is no improvement within one week, either the diagnosis should be reconsidered or some other anti-fungal agents should be tried.
This treatment with anti-fungal agents should be continued for at least one week more after the lesions have completely disappeared because otherwise there can be a recurrence.
When the lesion is in an eczematised state or it is likely to become eczematised, a combination of an anti-fungal agent with a topical corticosteroid should be used.
In case the lesion is lichenified, it is better to use hypertonic saline compresses or a keratolytic preparation over the lesion followed by local applications of a combination of an anti-fungal agent with a corticosteroid.
Read more about Eczema – Types, Causes, Risk Factors and Treatment
Systemic treatment
Systemic antifungal drugs are recommended in cases having tinea capitis, tinea barbae, tinea unguium, and generalized tinea corporis.
In tinea capitis, tinea barbae, and tinea unguium, the local anti-fungal agents are unable to penetrate to the sites where the fungus is located, while in generalized tinea corporis, it may be difficult and also uneconomical to use local anti-fungal agents.
In fungus infection of the palms and soles, particularly of the inter-digital region, it is usually quite difficult to eradicate the fungus with topical anti-fungal agents alone.
Thus, systemic drugs can also be used in patients which fail to respond to local anti-fungal agents.
Griseofulvin is a commonly used drug and is well-tolerated, but some patients develop headaches which may disappear within a few days even if the drug is continued. Occasionally, a patient may develop photo-sensitivity in which case, the drug must be withdrawn immediately.
Ketoconazole, fluconazole, isoconazole, miconazole, neticonazole, oxiconazole, sertaconazole, sulconazole, tioconazole and fosfluconazole are other systemic anti-fungal agents.
