Last Updated on August 18, 2023
Skin grafting is procedure of that transplants skin tissue from donor site, to the recipient site for reconstructing a defect in the skin.
Most of the skin grafting tissues are autografts.
An autograft is tissue transferred from one location to another on the same patient.
An isograft is tissue transferred between two genetically identical individuals.
An allograft is tissue transferred between genetically different members of the same species.
A xenograft is tissue transferred from a donor of one species to a recipient of another species.
Skin grafts are split-thickness skin grafts and full-thickness skin grafts.
Split-thickness skin grafts may be subdivided into thin (0.008- to 0.012-mm), medium (0.012- to 0.018-mm), and thick (0.018- to 0.030-mm) grafts.
These are discussed below.
Split Thickness Skin Grafts
Split-thickness skin grafts are most commonly used. It is used in areas where cosmesis is not a primary concern or the defect to be corrected is of a substantial size [precluding the use of an full thickness skin graft]
Split thickness skin graft is also called partial-thickness skin graft. It consists of epidermis and a variable thickness of dermis.
There remains some dermis on the donor site that heals by epithelialization from the cut ends of hair follicles and sweat glands in a manner similar to the healing of a graze or a superficial burn.
It is used in following situations
- Coverage of chronic skin ulcers
- Temporary coverage to allow observation of possible tumor recurrence,
- Surgical correction of depigmenting disorders
- Coverage of burn areas
- Accelerates wound healing
- Reduce fluid loss.
The thigh, is most frequently used as a donor site, but almost any site can be used. Grafts are harvested using a skin graft knife or a power dermatome. These consist of a blade and a guard that can be adjusted to determine the thickness of the graft.
Partial-thickness grafts are used to resurface relatively large areas of skin defect and are particularly useful in burns .
The use of split thickness skin graft is contraindicated in
- Areas where cosmesis matters
- When significant wound contraction could compromise function.
- Poor color and texture match
- Lack of pilar and eccrine adnexal structures
Full-thickness Skin Grafts
Full-thickness grafts consist of epidermis and all of the dermis. As the graft is full thickness, the donor site will not epithelialize and must be closed. Suitable donor sites are postauricular, supraclavicular and groin. Full-thickness grafts are most commonly used in repairing defects on the face.
Grafts taken from above the clavicles retain the ability to blush and can provide a very good colour match for facial skin, whereas grafts from below the clavicles will tend to look pale.
The use of full thickness skin grafts is indicated
- Defects in areas where the adjacent tissues are immobile or scarce.
- The tissue has premalignant or malignant lesions and precludes the use of a flap.
- When a multistaged procedure is inappropriate for the patient
- Punch grafting for hair transplantation
- Punch grafting for the surgical correction of depigmenting conditions
Nasal tip, helical rim, forehead, eyelids, medial canthus, concha, and digits are the areas where full thickness grafts work well.
The use of full thickness is contraindicated when the recipient bed, due to lack of reasonable vascular supply, cannot sustain the graft.
Uncontrolled bleeding in the recipient bed is another contraindication to the placement of a full thickness skin graft because hematoma and/or seroma formation.
Physiology after Skin Grafting
The harvested skin graft is completely devoid of its vascular supply prior to its transplantation in the recipient site.
All skin grafts initially adhere to the recipient bed by the formation of fibrin. Oxygen and nutrients diffuse through by a process known as plasmatic imbibition to keep the graft alive.
This occurs within the first 24-48 hours after the placement of the graft on the recipient bed.
Plasmatic Imbibation
During this process, the donor tissues receive their nutrition through the absorption of plasma from the recipient wound bed via capillary action.
In this phase, the graft is white and may appear somewhat swollen. Furthermore, because nutrients can be absorbed more effectively over shorter distances, thinner grafts tend to survive better in this stage of graft healing.
In addition, during this phase of healing, a fibrin network is created between the graft and the recipient bed. The recipient bed then generates vascular buds that grow into the fibrin network.
Inosculation
It starts 48-72 hours after grafting and may continue for as long as 1 week after grafting. During this time, the aforementioned vascular buds anastomose with both preexisting and newly formed vessels. This occurs more rapidly in an split skin graft than in a full thickness skin graft.
Lymphatics develop in the graft tissue at approximately 1 week after transplantation, and reinnervation of the graft may begin as early as the first few weeks, although many grafts may have some degree of permanent anesthesia.
In an avscular area with a small defect, the phenomenon of vascular bridging may be seen.
Here, vascular ingrowth occurs from the relatively highly vascularized lateral aspects of the recipient bed and bridges across the avascular base of the recipient bed.
For bridging to occur, the surrounding area must be quite vascular and the recipient area must remain small.
Procedure of Skin grafting
Split-thickness skin grafting
The recipient defect is measured accurately. Where possible a purse-string suture may around the defect reduce its overall size, which reduces the size of the donor graft required for coverage.
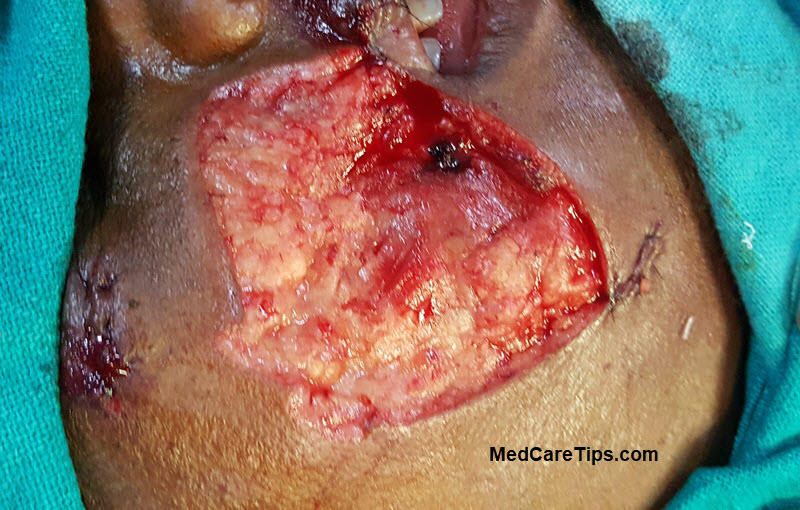
An appropriate donor site is chosen. Most commonly thigh is used. All surfaces of thigh except anterior can be chosen. Buttock or the medial aspect of the arm are other sites. The donor sites may vary depending on the size of the graft required to be harvested.
For example postauricular region is an excellent site for harvesting small to moderate-sized STSGs (< 10 cm) for the head, neck, and upper chest.
Depending on the area to be harvested the procedure can be carried under local anesthesia or regional anesthesia.
The donor site is prepared.
Graft can be harvested using manual instruments or power instruments.
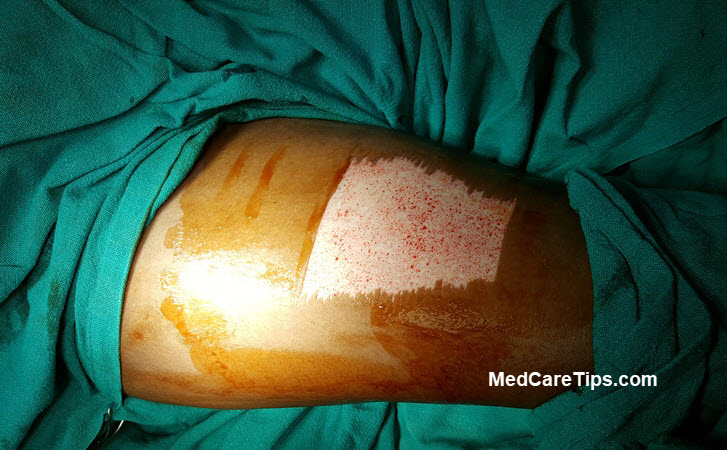
The manual instruments include
- Freehand dermatomes [Not typically used to harvest larger split thickness skin graft.]
- Scalpel blades
- Double-edged blades (Gillette blade)
- Weck knives
- Powered dermatomes
- Battery-operated [Davol]
- Alternating current (AC) operated [Padgett]
- Compressed water-pumped
- Nitrogen-driven [Zimmer]
Some dermatomes allow the surgeon to adjust the graft thickness and width whereas in others that is operator dependent.
After preparation, the donor site is lubricated with normal saline or mineral oil, a flat scale or sterile tongue depressor is kept across the donor site immediately in front of the dermatome cutting surface to provide a flat surface
The dermatome is pressed to the donor site with consistent light pressure, holding the device at a 30-45° angle to the skin surface and the harvested skin from the dermatome by using gentle traction.
The newly harvested graft is placed in sterile saline solution.
Usually the next step is meshing or creating fenestration. Some small grafts can be placed directly.
For meshing, a scalpel is often used to create multiple small slits or fenestrations to allow for drainage of serosanguineous fluid and accommodate minor expansion of the graft when applied to recipient site.
Meshing can also be done with help of a graft-meshing machine. After meshing, the graft is secured in place by using either staples or sutures.
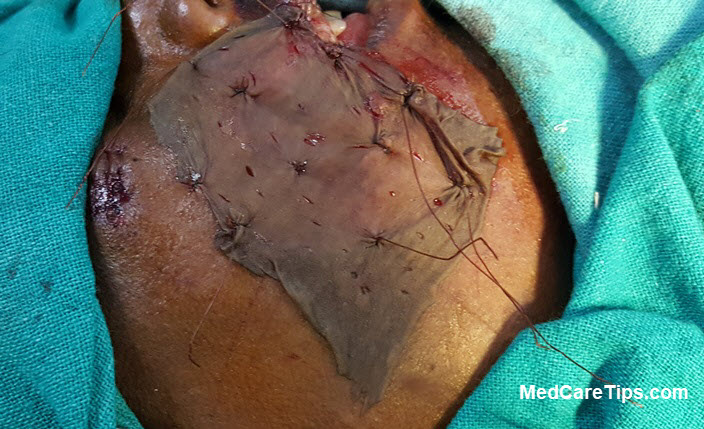
For dressing, a bolster may be applied to aid in graft apposition to the recipient bed, to decrease shearing forces, and to maintain a moist environment for the graft.
A pressure dressing over a nonadherent dressing applied directly over the graft is another alternative.
An occlusive dressing is done at the donor site for about 21-28 days.
Full-thickness skin grafting
Donor site is matched for color, texture, and sebaceous qualities similar to those of the area surrounding the defect as far as possible.
Common donor locations for full thickness skin grafts include areas of preauricular and postauricular, conchal bowl, supraclavicular, upper eyelid, nasolabial fold, axillary, antecubital, and inguinal fold skin.
Any redundant skin that is removed in the planning and reconstruction of the defect an also be source of full thickness graft.
Size must be measured accurately. Templates [foil or gauze] may be used.
In most cases, the tissue is removed with an elliptical incision that can easily be closed primarily.
The donor graft tissue is placed in sterile saline solution.
The graft can remain viable for as long as 24 hours after harvesting if it is refrigerated or kept on ice.
After harvesting the graft, the defect should be closed, and the the graft defatted by removing adipose tissue with scissors.
Contouring of the graft may be done.
The graft is fixed into place by interrupted sutures.
A of a tie-over bolster dressing can be used to provide firm apposition between the graft and the bed, decreases potential shearing forces and prevents the patient from manipulating the graft.
Complications of skin grafting
Infection
Infection is rare but risk is higher diabetes, those with immunosuppression, and those in whom the intraoperative time is prolonged.
Seroma and/or hematoma
Inadequate pressure dressings, trauma to graft and vigorous activity leads to higher risk of seroma or hematoma. NSAIDs, Coumadin, alcohol, or vitamin E, also may contribute to postoperative hematoma or seroma formation.
Graft Contracture
It is more common in split thickness skin grafts and can lead to cosmetic and functional problems.
Important Points
Graft take is only possible at well-vascularised recipient sites. Grafts will not take on bare bone, bare tendon or cartilage, but can survive on periosteum, paratenon and perichondrium.
In mobile areas appropriate splintage must be used.
Limbs that have been grafted should be elevated to reduce venous pressure during the process of revascularisation.
Grafts may heal with a mismatch in texture, color, or topography, and surgical correction can be considered at 6 weeks to 6 months after grafting.
Vascular lasers are used to soften healing graft scars and decrease their visible vascularity.
Gentle massage may soften and reduce elevated or firm scar tissue.
References
- Smahel J. The healing of skin grafts. Clin Plast Surg. 1977 Jul. 4(3):409-24.
- Evangelista MS, Kim EK, Evans GR, et al. Management of skin grafts using negative pressure therapy: the effect of varied pressure on skin graft incorporation. Wounds. 2013 Apr. 25(4):89-93.
- Lineen E, Namias N. Biologic dressing in burns. J Craniofac Surg. 2008 Jul. 19(4):923-8.
- Mirastschijski U, Bugdahl R, Rollman O, et al. Epithelial regeneration from bioengineered skin explants in culture. Br J Dermatol. 2006 Jan. 154(1):42-9. .
- Donohue KG, Carson P, Iriondo M, et al. Safety and efficacy of a bilayered skin construct in full-thickness surgical wounds. J Dermatol. 2005 Aug. 32(8):626-31.
- Futoryan T, Grande D. Postoperative wound infection rates in dermatologic surgery. Dermatol Surg. 1995 Jun. 21(6):509-14.
