Last Updated on April 9, 2019
Sinus
A sinus in Latin stands for a hollow or a bay or gulf. It is a blind track leading from an epithelial surface into the surrounding tissues. The track is often covered with granulation tissue.
It can be congenital or acquired.
A preauricular sinus is an example of congenital whereas sinus due to infection is an example of the acquired.
Acquired usually represents the path by which the discharge escapes from a cavity that has not closed yet and persists until the obstacle to the closure of the original abscess is removed.
It could be a foreign body [sequestrum, an infected ligature, or a bullet etc]. The removal of the foreign body causes healing.
The presence of a foreign body is often suggested by a mass of redundant granulations at the mouth of the sinus.
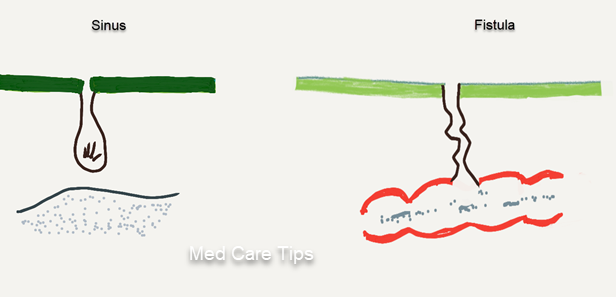
Fistula
Fistula in Latin stands for a pipe or tube. It is an abnormal communication between lumen or surface of one organ and lumen or surface of another organ.
Thus a fistula connects mucous surface to the skin or to another mucous surface.
Fistulae can result following suppuration, which normally occurs near the natural openings of mucous canals. Fistula from salivary gland on the cheek, lachrymal fistula besides the inner angle of the eye, a mastoid fistula near the ear etc.
Intestinal fistulae may occur in intestinal obstruction, after the strangulated hernia, tuberculous peritonitis, and other conditions.
Stricture of the urethra may lead to perineal fistula.
Congenital fistulae, such as occur in the neck from imperfect closure of branchial clefts, or in the abdomen from unobliterated fœtal ducts such as the urachus or Meckel’s.
Fistula can be congenital or acquired.
- Congenital fistulae arise from remnants of embryonic ducts that persist branchial fistula, Tracheo-esophageal fistula, congenital arteriovenous fistula and thyroglossal fistula
- Acquired fistula are secondary to the presence of foreign body, necrotic tissue in the affected area (or) microbial infection (or) following inadequate drainage of the abscess.
Causes of acquired fistulae are
Traumatic
- After intestinal fistulas
- Faecal
- Biliary
- Pancreatic
- Vaginal fistulae following instrumental delivery or difficult labour
- Vesicovaginal
- Rectovaginal
- Ureterovaginal fistula
- Infection/Inflammation
- Intestinal actinomycosis
- Tuberculosis
- Malignancy
- Iatrogenic
- Ateriovenous fistula for hemodialysys
Fistula could open externally as in orocutaneous, enterocutaneous, appendicular and thyroglossal fistula.
These could also open internally as in tracheo-esophageal, colovesical, rectovesical, arteriovenous fistula and cholecystoduodenal fistula
Causes of Persistence of a Sinus or Fistula
Foreign Body
A foreign body or necrotic tissue like a suture, hairs, a sequestrum, a faecolith or even a worm can cause persistence of these.
Inefficient Drainage
Long, narrow, tortuous track predisposes to inefficient drainage. So does the nondependent drainage.
Persistent Obstruction
In some cases, the fistula develops because the lumen is closed distal to the fistula. This leads to persistence drainage. In such cases, it is essential that the distal obstruction must be removed. In most of the cases, the fistula closes spontaneously.
High Pressure
In fistula-in-ano due to the normal contractions of the sphincter force fecal material through the fistula. This leads to persistence of fistula.
Changes in Lining
Epithelial or endothelial lining of the fistula/sinus prevents the closure. Dense fibrosis prevents contraction and healing.
Lingering infection/Disease
Some infections are known to be associated with sinuses. For example tuberculosis or actinomycosis. In cases of osteomyelitis, an active sinus indicates an ongoing infection.
A malignant disease may also cause persistence sinuses.
Similarly, ischemia of the tissue, drugs like steroids, cytotoxic drugs, malnutrition or radiotherapy may contribute.
Parasitic Infection
Guinea worm is the parasite responsible for the disease causing a persisting sinus on the lower leg.
Clinical Presentation
Often these are asymptomatic but can present with a recurrent or persistent discharge. They can be painful and may have constitutional symptoms if any deeply seated origin.
Electrolyte imbalance may occur due to loss of electrolytes in enteral fistulae.
Examination of sinus or fistula is very important in most of the cases.
Following are distinct features of different sinuses
- Multiple sinuses are seen in HIV patients or actinomycosis
- Sprouting granulation tissue in the opening suggests a foreign body
- Sinus flushing with skin is likely to be tubercular
- Excoriation may occur in those draining fecal matter or urine.
- Discharge
- White thin caseous, cheesy like- TB sinus
- Fecal- fecal fistula
- Yellow sulfur granules- actinomycosis
- Bony granules- osteomyelitis
- Yellow purulent- staph. infections
- Thin mucous like- brachial fistula
- Saliva- parotid fistula
Palpation reveals temperature and tenderness. Discharge may be seen after application of pressure over the surrounding area.
Chronic fistulae or sinuses may have induration.
Deeper lesions may become fixed.
Surrounding lymph nodes may be palpable.
Lab Studies
Routine blood test like CBC, ESR, CRP, and others as necessary are done.
Evaluation of discharge material is done by
- Culture/Sensitivity
- Cytology
- Gram staining
- AFB
- X-ray [to rule out underlying bony involvement]
- Biopsy
- CT Sinusogram to know origin and extent
- Fistulography or sinugraphy tells about the extent/origin of sinus or fistula. In this water-soluble or ultra fluid lipoidal iodine dye [poppy seed oil containing 40% iodine.
Treatment
Antimicrobials are given to treat infectious causes of the sinus. A number of sinuses close after infection is treated especially tubercular and fungal infections.
The affected part is rested. A foreign body if present should be removed.
Excision of the sinus may be required in certain cases.
Actual procedure and extent would vary with the individual cause.
In the case of osteomyelitis, sequestrum removal is done.
For treatment of fistula, the alternate draining route is created so that factor leading to persistence of fistula are removed.
