Last Updated on October 29, 2023
What Are Side Effects of Corticosteroid Therapy
Corticosteroids are very effective drugs in controlling the disease process but have potential for many side effects also. Most of the side effects are reversible and the patient is expected to revert back to the normal state after the treatment has been completed and the corticosteroids have been withdrawn.
Even when the side effects are serious, the effect of the side effect has to be evaluated in comparison with the seriousness of the disease being treated.
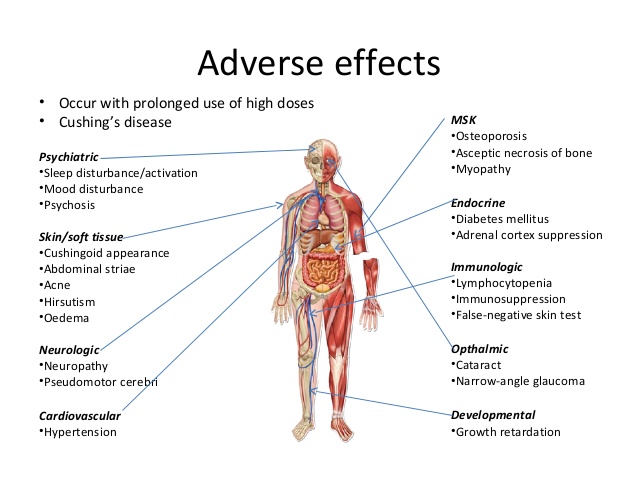
Following are the major side effects seen during therapy with corticosteroids along with the suggestions for their prevention and treatment.
Electrolyte imbalance
Most corticosteroids lead to retention of sodium in the body and excretion of potassium. This can lead to a feeling of extreme weakness, vomiting and even sudden death due to stoppage of the heart.
To prevent this, every patient who is given a dose higher than 20 mg of prednisolone a day, should be put on a salt-free diet and given additional amounts of potassium. Potassium can be given either in the form of potassium chloride or as potassium citrate.
One gm of either of these in powder form or as a mixture, for every 10 mg of prednisolone, to a maximum of 4 to 5 gm a day is, as a rule, sufficient. One should, however, check the levels of sodium, potassium and chloride in the serum once or twice a week and make changes in the therapy whenever indicated.
Pulse therapy corticosteroids do not lead to electrolyte imbalance.
Increased susceptibility to infections
Treatment with corticosteroids makes a patient very susceptible to infection. It is therefore, quite necessary to keep these patients under strict vigilance, particularly those having treatment with higher doses.
If at any time concomitant infection is discovered, the patient must be treated with appropriate anti-infective agents. It has also been observed that patients who had an old healed lesion of tuberculosis in the lungs, may show reactivation of tuberculosis.
Susceptibility to infections is more severe in patients treated with pulse therapy, especially if the patient is being given immuno-suppressive drugs as well.
Increase in body weight
Corticosteroids lead to an increase in appetite and deposition of fat on the face and trunk, resulting in the characteristics moon facies and the buffalo-type obesity. This is one of the commonest side effects and the only way to counter this is to restrict the calorific value of the patient’s diet.
This can be achieved by advising the patient to depend mostly on vegetables, pulses and salads and take as less of chapattis, rice and milk as possible. This obesity, however, is quite innocuous and disappears soon after treatment with corticosteroids is stopped.
Pitting edema
Patients on high doses of corticosteroids also tend to develop pitting edema due to the retention of sodium in the body. Whenever it appears, it should be treated with diuretics, but those which lead to excretion of potassium should be avoided.
Peptic ulceration
Corticosteroids increase the tendency of the patient to develop peptic ulcers. Occasionally, perforations of the stomach leading to a fatal termination have been observed in patients even without any clinical evidence of gastric ulcer.
Increased tendency for diabetes mellitus
Corticosteroids are well known to lead to hyperglycaemia and worsening of the diabetic state if it already exists or making a patient manifest diabetes if there is a tendency for it. It is therefore, worthwhile testing the patient’s urine for sugar and if necessary, the blood as well for periodic evaluation of the diabetic state, particularly if he is one high dosage schedules.
Presence of diabetes in the patient does not contra-indicate therapy with corticosteroids, but additional measures must be instituted for the control of the diabetic state. Once treatment with corticosteroids is stopped, the diabetic state also tends to return to the normal state.
Hypertension
Retention of sodium and water in patients having treatment with corticosteroids can also result in a rise in the blood pressure.
If the hypertension is mild, it may be easily controlled by restricting salt in the diet, and by diuretics; but in case it is severe, the patient may have to be given tranquillisers or even anti-hypertensive drugs.
Osteoporosis
Treatment with corticosteroids leads to a marked loss of proteins from all over the body, but particularly from the bones, along with decalcification. This may result in pains in the bones or even pathological fractures, more so, if the patient is on a long term high dosage schedule.
Steroid acne
In some patients, corticosteroids produce a hyperkeratosis of the follicular openings leading to the appearance of follicular papules on face or upper trunk. Usually, these lesions are non-inflammatory and do not produce comedones but sometimes they may be inflamed as well. They disappear when the treatment with corticosteroids is stopped, but in case they are troublesome, they should be treated in the same manner as ordinary acne.
Striae atrophicans
Some patients develop large, linear atrophic areas on their skin resembling those seen on the abdomen of females during pregnancy. These striae usually appear in those individuals who put on weight rapidly and at those areas which are subjected to tension. Once the striae have appeared no treatment can make them disappear although with time, the striae become less prominent.
Increased tendency for bleeding
Very occasionally, some patients develop spontaneous haematomas or ecchymosis in their skin. This is due to the fact that the connective tissue support of small blood vessels becomes weak due to corticosteroid therapy.
Therefore, minor traumata which usually go unnoticed, may lead to rupture of the blood vessels and result in ecchymosis. There is no need for any treatment for ecchymosis because these disappear spontaneously.
Congenital abnormalities
When given to pregnant women corticosteroids can interfere with the development of tissues and organs of the foetus and thus lead to congenital abnormalities. These can also lead to a still-birth. They should therefore, be avoided as far as possible in pregnant women, particularly during the first three months of pregnancy.
Myopathy
Most patients on prolonged corticosteroid therapy complain of weakness in the muscles. The total muscles mass becomes reduced, the limbs become thin and the patient finds it difficult to sit up or walk. These changes are more common with some corticosteroids such as triamcinolone as compared to others.
Cataract
Posterior subcapsular cataracts and glaucoma are common complications involving the eye.
Hypertrichosis
Increased growth of coarse hairs on the forehead and sides of face is also seen in some cases. This is also reversible when the corticosteroids are withdrawn.
