Last Updated on October 29, 2023
Molluscum contagiosum is a viral infection of the skin or occasionally of the mucous membranes. This condition is also known as water warts. It is caused by a DNA poxvirus called the molluscum contagiosum virus. Molluscum contagiosum virus is the largest virus affecting human beings. This is a cytoplasmic virus that gets implanted on the skin by contact with other infected individuals.
The disease is common in children, though less commonly, it may also occur in adults. The incubation period is 2-7 weeks.
The larger lesions tend to become umbilicated in the center.
As the old lesions heal spontaneously in 1-2 weeks, the new lesions can continue to appear by auto-inoculation. Most often, there are only a few lesions.
Widely disseminated lesions may occur in atopic patients or those with suppressed cell-mediated immunity. When present in the genital area, molluscum contagiosum may be transmitted through sexual contact.
Molluscum contagiosum virus belongs to the Poxviridae family and six serotypes have been identified. More than 95% of infections are caused by type 1.
Most of the molluscum infections in HIV are caused by type II virus.
Molluscum contagiosum forms 1% of all diagnosed skin disorders. Though the virus is seen worldwide, it is more prevalent in tropical areas.
Males are more affected by molluscum contagiosum.
The infection is rarely seen in children younger than age 1 year.
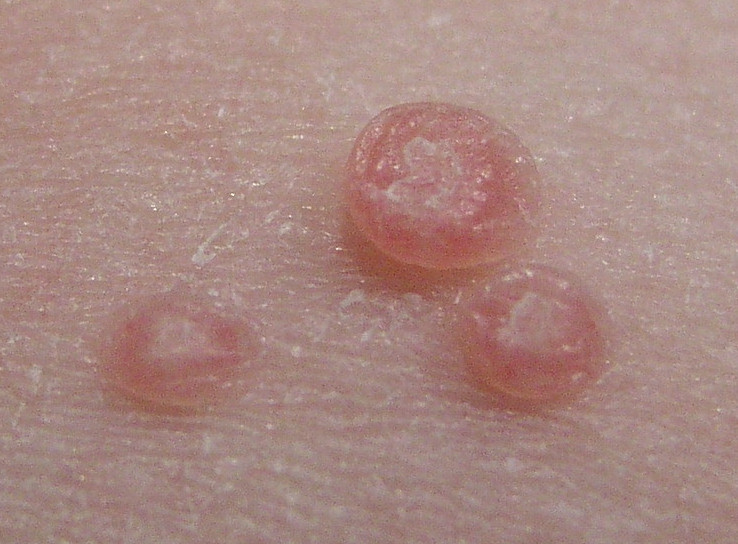
Different Disease Patterns of Molluscum Contagiosum
The disease has different profiles depending on the patient population
The prognosis and therapy are different for each of these groups. These groups are children, healthy adults, and immunocompromised people.
In children, the spread occurs by direct skin-to-skin contact or indirect skin contact with fomites – bath towels, sponges, and gymnasium equipment.
The lesions are seen on the chest, arms, trunk, legs, face, axillae, and intercrural region.
Mucous membranes of the lip, tongue, and buccal mucosa may be involved but are less common.
There is sparing of the palms.
In immunocompetent adults, the most common transmission of molluscum contagiosum in adults is sexual.
The lesions are spread over the perineum, genitalia, lower abdomen, or buttocks.
Both in children and adults, the disease is often self-limiting.
In immunocompromised patients [as in AIDS] the disease is more severe and also resistant to treatment.
Multiple sexual partners and unprotected sex may increase the risk.
Other than HIV infection, following immunocompromised persons could get affected.
- Sarcoidosis
- Lymphocytic leukemia
- Immunodeficiency disorders
- Thymoma
- Patients on steroids
- Patients on methotrexate
- Disseminated malignancy
The Course of Molluscum Contagiosum Infection in Body
There are 2-7 weeks of incubation period but a latent period of as long as the half-year is known.
The virus infects the epidermis and divides in the cytoplasm of epithelial cells. This leads to the enlargement of the cells and the formation of cytoplasmic inclusions.
Cellular proliferation produces lobulated epidermal growths. These growths compress epidermal papillae. The basal layer remains intact.
Cells at the center of the lesion show the greatest distortion. Ultimately, these cells are destroyed and this forms large hyaline bodies called molluscum bodies or Henderson-Paterson bodies. These contain cytoplasmic masses of virus material.
These bodies appear as white depression at the center of the lesion leading to the umbilicated appearance of the lesion.
Occasionally, inflammatory changes may occur.
The virus evades the immune system by producing virus-specific proteins.
Cell-mediated immunity is involved in curtailing and fighting this disease.
The virus is weakly immunogenic and antibody formation is not frequent.
Most of the cases resolve without therapy within 6-9 months, some persist for 3-4 years. Individual lesions seldom persist for more than 2 months.
Patients with HIV or those receiving prednisone, methotrexate, or other immunosuppressive medications may have more extensive and resistant infections.
The severity of infection is inversely related to the CD4 cell count.
Symptoms and Signs of Molluscum Contagiosum Infection
Systemic symptoms like fever, malaise, and nausea, etc. are not seen.
The lesions can be tender or itchy.
A history of contact should be looked for. Direct contact or sharing of gym equipment or benches etc. In adults, sexual history should be sought.
One of the peculiar features of this disease is the development of lesions along the scratch line. This occurs due to a phenomenon called autoinoculation.
Patients with atopic dermatitis may have extensive disease.
Lesions are dome-shaped and flesh-colored papules with a central umbilication [may not always be ovbious].
Lesions are usually 2-5 mm. In extensive infections, giant lesions up to1.5 cm may be seen.
Children and normal adults have less than 20 lesions but immunocompetent may have way more.
Beneath the umbilicated center is a white, curd-like core [ contains molluscum bodies].
Lesions may confluent to form a plaque.
In children, the lesions are seen on the face, trunk, and extremities, and palms are generally spared. Rarely, the soles, oral mucosa, or conjunctiva may be affected.
The lesions may occur in the axillae and intercrural region. If the patient has atopic dermatitis, the number of lesions could be more. About a tenth of the patients may develop eczema around the lesions.
Read more about Eczema – Types, Causes, Risk Factors, and Treatment
Some of the lesions may show inflammatory changes evidenced by suppuration, crusting, and eventually resolution.
In sexually transmitted cases, the perineum and surrounding areas are affected.
In immunocompromised persons, the distribution could be extensive.
Facial and perioral molluscum contagiosum could be manifestations of HIV infection.
Complications
- Inflammation
- Secondary infection of the lesion
- Cellulitis
Differential Diagnoses
- Condyloma Acuminatum (Genital Warts)
- Cryptococcosis
- Pearly Penile Papules
- Pediatric Keratosis Pilaris
- Pediatric Milia
- Pediatric Pyogenic Granuloma
- Varicella-Zoster Virus (VZV)
Diagnosis
The distinctive, central umbilicated dome-shaped lesion often leads to a straightforward diagnosis.
A biopsy may be done if there is uncertainty in the diagnosis.
Histologic examination characteristic intracytoplasmic inclusion bodies (molluscum bodies, or Henderson-Paterson bodies) are seen on histologic examination findings.
- Thickening of epidermis
- Henderson-Paterson bodies
- Intracytoplasmic, eosinophilic, granular inclusions within the keratinocytes of the basal, spinous, and granular layers of the epidermis.
- can measure 35µm in diameter.
- Ultrastructural studies have shown that these bodies are membrane-bound sacs that contain numerous molluscum contagiosum virions [as seen on ultrastructural studies]
- An inflammatory dermal infiltrate may be seen in few cases
Another method to look for Handerson Paterson bodies is a microscopic examination of cellular exudate.
Polymerase chain reaction (PCR) assay can be used to detect and categorize the molluscum contagiosum virus in skin lesions.
The patient is evaluated for other sexually transmitted diseases to rule out other STDs. Always consider testing for HIV infection in patients with facial lesions.
Treatment of Molluscum Contagiosum
Molluscum contagiosum is generally self-limited and heals spontaneously after several months. A lesion usually does not last more than two months.
Four main treatment approaches can be used in Molluscum contagiosum
Do Nothing
Also called benign neglect or skillful neglect, nothing active is done and the lesions are monitored. It is more appropriate in children and when required minor intervention may be done [lesional trauma]. Sometimes individual lesions may be intervened to control autoinoculation and contact spread of the disease.
Direct Lesional Trauma
Minor trauma to the lesions leads to produces an inflammatory response and resolution of the lesion.
This can be done by topical caustic agents like cantharidin, tretinoin, bichlor and trichloroacetic acid, salicylic acid, lactic acid, glycolic acid, silver nitrate, potassium hydroxide and dilute povidone-iodine.
[None of these caustic agents has been approved by the FDA for the treatment of molluscum contagiosum.]
Physical trauma can be done by
- Rupture of the central core with a needle or a toothpick or tweezers
- Can be done as a home remedy for molluscum contagiosum.
- Take out the central firm core of lesions using a clean needle or a toothpick.
- This irritates the lesion and resolves in 7-14 days
- The lesion can be expressed by tweezers also.
- Curettage
- In-office procedure
- Lesions are curetted with a sharp curette
- Shaving the lesion with a scalpel
- Electrodesiccation
- Passing a very low current through the lesion to desiccate
- Cryotherapy
- Freezing the lesion by pressurized liquid nitrogen
- Could be painful
- Pulsed dye laser
- Very high single sitting treatment success rate
In patients with AIDS, two or more modalities may be combined.
Immune Response Stimulation
- Intralesional interferon-alfa
- Topical injections of streptococcal antigen
Antiviral Therapy
In immunocompromised patients, antiviral therapy improves lesions.
- Ritonavir
- Cidofovir
- Zidovudine.
References
- Connell CO, Oranje A, Van Gysel D, Silverberg NB. Congenital molluscum contagiosum: report of four cases and review of the literature. Pediatr Dermatol. 2008 Sep-Oct. 25(5):553-6.
- Braue A, Ross G, Varigos G, Kelly H. Epidemiology and impact of childhood molluscum contagiosum: a case series and critical review of the literature. Pediatr Dermatol. 2005 Jul-Aug. 22(4):287-94.
- Nageswaran A, Kinghorn GR. Sexually transmitted diseases in children: herpes simplex virus infection, cytomegalovirus infection, hepatitis B virus infection and molluscum contagiosum. Genitourin Med. 1993 Aug. 69(4):303-11.
- Cribier B, Scrivener Y, Grosshans E. Molluscum contagiosum: histologic patterns and associated lesions. A study of 578 cases. Am J Dermatopathol. 2001 Apr. 23(2):99-103.
- Nguyen HP, Franz E, Stiegel KR, Hsu S, Tyring SK. Treatment of molluscum contagiosum in adult, pediatric, and immunodeficient populations. J Cutan Med Surg. 2014 Sep-Oct. 18(5):299-306.
- Mathes EF, Frieden IJ. Treatment of molluscum contagiosum with cantharidin: a practical approach. Pediatr Ann. 2010 Mar. 39(3):124-8, 130.
- Niizeki K, Hashimoto K. Treatment of molluscum contagiosum with silver nitrate paste. Pediatr Dermatol. 1999 Sep-Oct. 16(5):395-7.
- Hammes S, Greve B, Raulin C. [Molluscum contagiosum: treatment with pulsed dye laser]. Hautarzt. 2001 Jan. 52(1):38-42.
