Last Updated on August 2, 2019
Lymphadenopathy means lymph nodes which are abnormal in size, number or consistency and is often used as a synonym for swollen or enlarged lymph nodes.
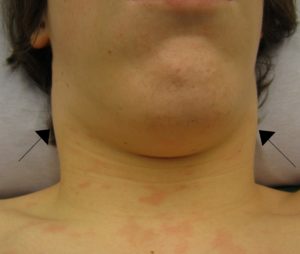
Image from Wikipedia under GNFL
Causes of Lymphadenopathy
Reactive
- Enlargement of lymph nodes in response to infection or injury somewhere in the body.
Inflammatory
- Lymphadenitis
- Bacterial infection
- Tuberculosis
- Filariasis
- Syphilis
- Lymphogranuloma inguinale
- AIDS
Malignancies
- Primary malignancies
- Hodgkin’s disease
- Non-Hodgkin’s lymphoma
- Secondary malignancies
- carcinoma
- sarcoma
- malignant melanoma
- Hematological
- Chronic lymphocytic leukemia
Immunological
- Serum sickness
- Drug reaction
- SLE
- Rheumatoid arthritis
Characteristics of Lymphadenopathy in Different Conditions
Reactive Lymphadenitis
- The lymph nodes are enlarged in response to infection or injury in the area drained by those lymph nodes.
- It is commonly seen in children as they develop immunity to different germs.
- Small, soft and movable lymph nodes
- Usually donot require treatment
Acute Lymphadenitis
- Enlarged, tender and fixed lymph nodes.
- The overlying skin may become red, hot and brawny.
- Primary infective focus may be found.
Chronic Septic Lymphadenitis
- Enlarged, slightly tender lymph nodes which may or may not be matted.
- If an abscess has occurred, fluctuation in the center and pitting on pressure at the periphery will be evident. It is often difficult to differentiate from tuberculous lymphadenitis.
Tuberculous Lymphadenitis
- Commonly affects the deep cervical, mesenteric and axillary lymph nodes.
- The lymph nodes may be discrete (when it resembles chronic septic lymphadenitis) or may be matted.
- If caseation has occurred, cold abscess results which may burst forming tuberculous ulcer or sinus which takes a long time to heal.
- Fever with chills, weight loss, anorexia, and respiratory complaints may be present.
Syphilitic Lymphadenitis
- Painless, firm, discrete and shotty glands which do not suppurate.
- In secondary syphilis, generalized lymphadenopathy occurs involving especially epitrochlear and occipital glands.
- Other evidence of syphilis with positive tests for syphilis like WR, VDRL, TPI, and FTA ABS.
Filarial Lymphadenitis
- Pain, tenderness, and swelling of the inguinal lymph nodes, spermatic cord, and scrotum.
- Lymphangiectasia (dilation of the lymph vessels) of the inguinal region and spermatic cord.
- Eosinophilia and microfilaria can be demonstrated in the blood.
- Lymph node biopsy may reveal an adult worm.
Lymphogranuloma Inguinale
- Suppurative lymphadenitis with ulceration, sinus formation and extensive scarring of the inguinal lymph nodes.
- Frei’s test is confirmatory.
Secondary Carcinoma
- The nodes are enlarged, irregular and fixed to all structures including the skin.
- Hard consistency.
- Primary growth may be detected.
- The patient may be cachectic and wasted.
Hodgkin’s Disease
- Bimodal incidence
- The first peak occurs in young adults (15-35 years)
- The second peak occurs in older people (> 55 years).
- Cervical glands are affected early but later all lymph nodes are involved.
- Lymph nodes are elastic and rubbery, discrete and movable with little tendency towards matting, softening or suppuration.
- Edema, venous engorgement, and cyanosis of head and neck may occur due to pressure on the superior vena cava and the bronchus by the mediastinal glands. Root pain and paraplegia may develop due to pressure on the spinal cord.
- Hepatomegaly, splenomegaly, and anemia occur.
- Weight loss of more than 10% of body weight and night sweats.
- Peripheral smear will show lymphocytosis and eosinophilia.
- Lymph node biopsy shows characteristic Reed Sternberg cell.
Non-Hodgkin’s Lymphoma
Similar to Hodgkin’s lymphoma in clinical presentation except
- Enlargement of nodes in Waldeyer’s ring and supratrochlear glands
- Symptoms are less common
- Can be a manifestation of HIV infection
- Diagnosis is confirmed by histological examination (biopsy) of the involved lymph node.
Infectious Mononucleosis
- Acute onset of fever, sore throat, headache, malaise and tiredness
- The lymph nodes are enlarged, discrete and slightly tender affecting especially the cervical and submandibular nodes.
- Non-tender splenomegaly may occur.
- A petechial rash may occur at the junction of soft and hard palate on the fourth day and may persist for 3-4 days.
- Peripheral smear shows leucocytosis (absolute lymphocyte count more than 1500/c mm) with atypical lymphocytosis.
- Paul-Bunnell test may be positive in 1:32 dilution or more usually in the first 10 days.
Location and Examination of Lymph Nodes
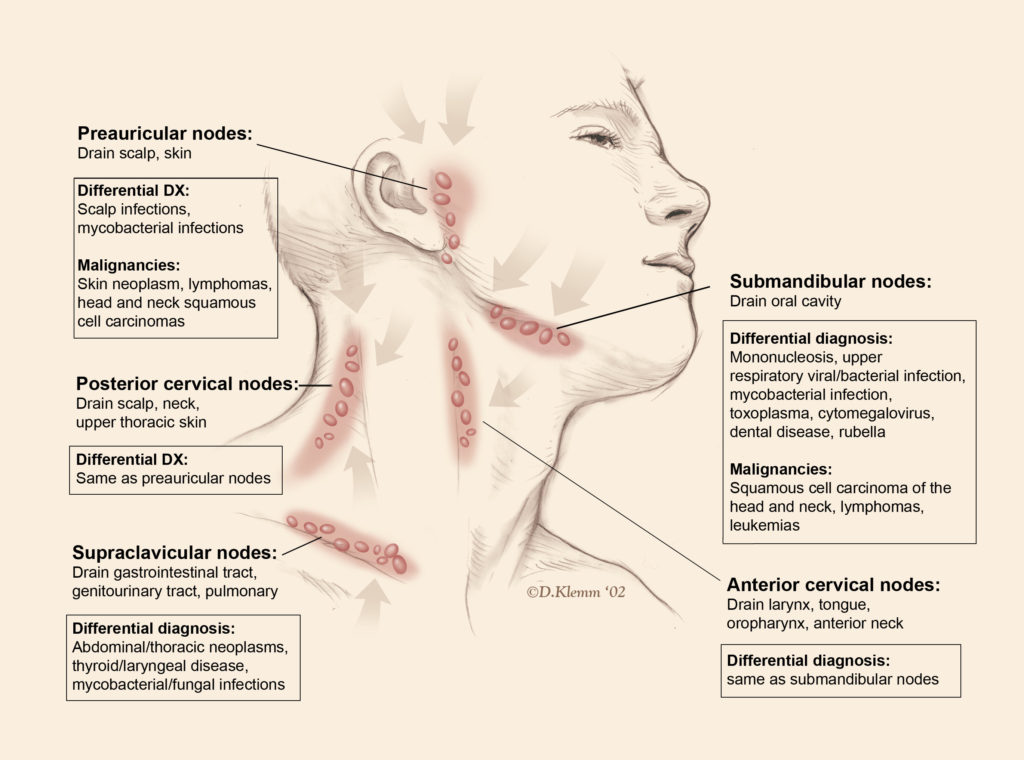
Cervical Lymph Nodes
The lymph nodes of the neck should be examined by standing behind the patient with the patient’s neck slightly flexed. The nodes must be examined from above downwards-submental, submandibular, tonsillar, cervical, posterior auricular and occipital groups.
In the left supraclavicular fossa, a lymph node may be palpable (Virchow’s node) which occurs due to metastasis from the stomach or testicular malignancy.
Axillary Lymph Nodes
The axillary glands should be examined by inserting the fingers in the axilla with the patient’s arm slightly abducted. The arm is then abducted and the apical, anterior, posterior, medial and lateral groups of lymph nodes are examined.
Supratrochlear Lymph Nodes
The supratrochlear lymph nodes are palpated on the medial aspect of the arm between the groove of biceps and brachialis muscle an inch above the arm-fold.
Inguinal nodes
The inguinal nodes are examined in the supine position with the thigh extended. Both the medial and lateral groups of lymph nodes are examined.
Scalene nodes
Scalene nodes are present behind the sternomastoid muscle and may be palpable. In suspected malignancy, biopsy it taken from that area, even if the nodes are not palpable.
Examination of Swollen Lymph Nodes in Lymphadenopathy
Inspection
Most of the superficial lymph nodes are visible when enlarged. The site of lymphadenopathy often gives the clue to its cause. Tuberculosis often affects the upper deep cervical nodes, secondary syphilis affects supratrochlear nodes, carcinoma of stomach affects the left supraclavicular nodes whereas filariasis affects the inguinal nodes.
The skin overlying the lymph nodes may show redness indicating underlying inflammation. Ulceration or sinus may be present in tuberculosis.
Palpation
Raised temperature and tenderness are noted. If present, they suggest acute inflammation. The surface is smooth normally but matted in tuberculosis and irregular in malignancy and inflammation.
The consistency of the nodes is noted. Normally it is firm.
It is rubbery in Hodgkin’s disease, firm, and shotty in syphilis, matted in tuberculosis and hard in malignancy.
The mobility of the nodes is noted. Normally they are mobile and free from the skin. In certain inflammatory conditions and malignancy they may be fixed and non-mobile.
Lab Studies
- Complete blood count
- Peripheral blood film examination
- ESR
- Chest X-ray
- Tuberculin test
- LDH
- Uric acid
- FNAC
- Biopsy
Treatment of Lymphadenopathy
Most of the patients with lymphadenopathy are treated conservatively.
Antibiotics are used if a bacterial infection is suspected.
A biopsy is done sooner if a malignancy is suspected. FNAC is the usual first step. If it is positive for malignancy, further investigations should be considered and treatment plan is formed accordingly.
