Last Updated on October 29, 2023
Lungs are balloon like structures in the body whose purpose is gas exchange.
When we take our breath, called inspiration, atmospheric air enters the airways and travels to the alveoli, the smallest units of lung for air exchange. Oxygen diffuses from the alveolus through the alveolar-capillary membrane into the blood, and carbon dioxide diffuses from the blood into the alveolus. This is known as respiration.
During exhalation [breathing out], gas moves from the alveoli toward the upper airways and is exhaled through the mouth and nose into the atmosphere.
The exchange of air between the lungs and the atmosphere is known as ventilation.
This continuous process of ventilation and respiration depends on a patent airway system, intact pulmonary parenchyma, adequate blood flow to the lung and a normal neuromuscular system.
Anatomy of Lungs
Airways
The upper airways consist of the oral and nasal cavities, pharynx, and larynx. The primary function of the upper airways is to prepare the inspired air for entry into the lungs.
The nasal passages are particularly designed to act as an air conditioner. The nasal turbinates and mucous membranes in the nasal cavity warm filter, and humidify the inspired air during inspiration.
Filtering of the inspired air is accomplished in part by the strong hairs of each nostril. A rich network of blood vessels in the mucosal membrane helps in warming and humidifying the inspired air. The air is further warmed as it passes below.
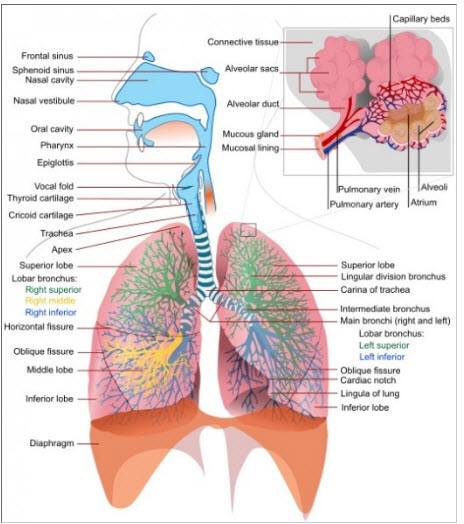
Below the larynx, the airways can be subdivided into three components
- Trachea, bronchi and ending with the terminal bronchioles. These are also called conduction airways and serve for passage of air
- Respiratory bronchioles where gas is conducted and some gas exchange occurs
- Alveolar ducts, sacs, and alveoli, where gas exchange takes place with the pulmonary capillary blood.
Tracheobronchial Tree
The trachea is about 2.0-2.5 cm in diameter and nearly 11 cm long in the adult.
It extends from the level of the 6th cervical vertebra to the 5th thoracic vertebra. The trachea divides into the right and left main stem bronchi at the level of the carina. The right and left main stem bronchi further subdivide into lobar bronchi, then into subsegmental bronchi.
The larger airways divide into even smaller airways similar to the branching of the roots of a tree. Collectively, the trachea and branching airways are commonly referred to as the tracheobronchial tree.
Each division or generation of airways continues dividing in the lungs. From the trachea to the alveoli the airways divides into approximately 23 generations or groups of branching airways in the adult.
Smooth muscle is located in the airways walls throughout most of the tracheobronchial tree although it varies in its location with the size of the airways. In the trachea and large bronchi, a band of muscle connects the opening of U-shaped cartilages that support the airways. As the airways size decreases, the smooth muscles become progressively more prominent with muscle fibers spiraling in both directions crisscrossing in the walls. Therefore, the effect of smooth muscle contraction is more significant distal to the trachea and large bronchi and will decrease airways diameter and length in these more peripheral airways. Smooth muscle is present to the level of the respiratory bronchioles.
Ciliated columnar epithelial cells line nearly all of the respiratory tract below the larynx to the level of the respiratory bronchioles. The cilia that border the columnar epithelium constantly undulate in a rhythmic pattern similar to what is seen as the wind blows over a wheat field. This process removes most of the particles and debris that enter the airways. The escalator-like action of these cells does an effective job of keeping the airways clean.
Bronchial and Pulmonary Circulation
Blood supply to the lungs can be divided into two components
- Bronchial circulation
- Pulmonary circulation.
Bronchial circulation serves to meet the metabolic demands of the lung tissue and is supplied by the aorta. Bronchial circulation supplies blood to and from the entire trachea-bronchial tree to the level of the terminal bronchioles.
The pulmonary circulation begins in the right ventricle and ends in the left atrium, and supplies blood to the respiratory bronchioles, alveolar ducts, and alveoli. Blood flow through the pulmonary circulation allows gas exchange to occur.
Some of the blood in capillaries of the bronchial and pulmonary circulation mix at the level of airways near the terminal and respiratory bronchioles.
Mechanics of Respiration
Thorax is a rigid structure to protect the vital organs that it contains but flexible and pliable enough to permit chest expansion with breathing.
The rigidity is provided by the bones, cartilage and supportive tissue. Various joints significant changes in size and shape. The 12 pairs of ribs provide the structural foundation of the chest.
During inspiration, the chest and lungs expand in all three planes: anteroposterior, transverse, and longitudinal. On the inhalation, the ribs move anteriorly, upward, and spread apart as a result of the contraction of the diaphragm and accessory muscles of inspiration.
Muscles of Respiration
Primary
Diaphragm is the primary muscle of respiration. It is composed of two dome-shaped hemidiaphragms that form the floor of the thorax and separate the thorax from the abdomen. During inspiration, the diaphragm contracts and flattens and descends toward the abdomen. Diaphragmatic contraction causes the longitudinal lung size to increase. During exhalation, the diaphragm relaxes and ascends while returning to its resting, dome-shaped configuration.
Accessory
These muscles assist the diaphragm in increasing, thoracic volume. These muscles are
- Sternocleidomastoid
- Trapezius
- Intercostal
- Rhomboid muscles.
During relaxed breathing accessory muscles are not active. They start participating in breathing with activity or when the resistance to air movement into the thorax is increased such as exercise.
The abdominal muscles usually do not participate actively in relaxed breathing; however, during forced exhalation, rapid breathing, exercise, coughing, or sneezing, the abdominal muscles play an important part in providing maximum function.
Mechanics of Lung Function
Lungs and surrounding chest wall form a ventilator apparatus that is similar in function to a pump. The chest wall and lungs are separated by the parietal and visceral pleura. The pressure in the pleural space in referred to as the pleural pressure and varies during breathing.
In the resting state, when there is no air flow in or out of the lungs, the airways resistance is zero and the pressure along the entire airway from the month to the alveoli is nearly equal to atmospheric pressure.
During the end of relaxed expiration, the lung recoils inwardly whereas the recoil of the chest wall is directed outwardly. These opposing forces generate a subatmospheric pressure of approximately 5 cm of water that varies in magnitude throughout each breathing cycle.
During inspiration, the diaphragm contracts and the lung expands leading to fall of pleural pressure below atmospheric pressure. The pressure gradient created between the airways opening of the mouth and alveoli causes air from the atmosphere to fill the lungs.
During the end or relaxed inspiration, the volume of air in the lungs increases and this causes pleural pressure and alveolar pressure to approximate atmosphere pressure and air flow into the lung stops. During exhalation, as the inspiratory muscles relax and the lung recoils, alveolar pressure exceeds pressure at the airways opening. The pressure gradient causes air to flow out of the lungs.
Physiology of Respiration
Lung Volumes and Capacities
Tidal Volume [TV]
The volume of air entering the lungs during inspiration and leaving during exhalation is the tidal volume.
Inspiratory Minute Volume or VI
The sum of all the inhaled air measured over a minute.
Similarly, the expiratory minute volume is the exhaled air over a minute.
Inspiratory Reserve Volume [IRV]
The maximum volume of air that can be inhaled after normal inhalation.
Inspiratory Capacity [IC]
The sum of the tidal volume and inspiratory reserve volume compartments comprise the inspiratory capacity. This represents maximal inhaled volume originating from the end of the resting exhaled tidal volume.
Expiratory Reserve Volume. [ERV]
The maximum volume of air exhaled further after the end of the normal tidal volume is the volume of air remaining in the lungs after maximal exhalation is the residual volume. [RV]
Functional Residual Capacity [FRC]
The sum of the expiratory reserve volume as the residual volume compartments.
Total Lung Capacity
The volume of air in the lungs following maximal inspiration is total lung capacity.
Vital Capacity
The maximal volume of air exhaled from the lungs after a maximal inspiration or the maximum volume of air inhaled following maximal exhalation is the vital capacity
Vital Capacity = Inspiratory reserve volume+ Tidal Volume + Expiratory reserve volume
The resting volume in the lungs can be altered many factors. As the lungs lose elasticity with aging, or with emphysema, the functional residual capacity increases. When lung expandability decreases, as in pulmonary fibrosis, the FRC decreases.
The FRC also decreases when there is a change from the erect position to the supine position [caused by impingement of the abdomen on the diaphragm]
Pulmonary Gas Exchange
The major function of the lungs is to provide oxygen to, and remove carbon dioxide from, the blood flowing through the pulmonary capillaries. During breathing, alveolar air and pulmonary capillary blood come into intimate contact separated only by a very thin alveolar-capillary membrane.
Blood leaving the right ventricle flows through the pulmonary capillaries richly perfusing the alveoli. Some of the oxygen leaves the alveoli and diffuses across the alveolar-capillary membrane into the blood while some of the carbon dioxide leaves the capillary membrane and diffuses into the alveoli.
The carbon dioxide that leaves the blood by the alveoli and the airways is exhaled into the atmosphere.
The oxygen is attached to hemoglobin throughout the body via the systemic circulation. Oxygen diffuses out of the systemic capillaries to the various tissues of the body.
Carbon dioxide, which is one of the byproducts of metabolism, diffuse out of cells into the systemic capillaries. Capillary blood transports the carbon dioxide to the lungs via the venous blood vessels, right atrium, and right ventricle.
Gas exchange takes place in the lungs as the blood reaches the pulmonary capillaries, thus completing the circulatory loop.
Lungs in Infants
The infant has several developmental differences in the structure and function of the lung. The lung develops and grows continuously from fetal life through childhood. The understanding of this growth and development of the lung is helpful to interpret the pulmonary signs identified by physical examination.
Anatomy
There is little change in the topography of the lung from fetus to infant to adult. However, the external chest wall changes its shape from being round to ovoid in the transverse plane.
The cross-sectional area of the thoracic cavity in the adult is fairly equal from base to apex. Whereas, the infant’s cross-sectional area is much larger at the base than at the apex making the infant’s chest appear more bell-shaped.
The trachea of the newborn is funnel-shaped, wider at the infant larynx and more narrow toward the carina. It becomes cylindrical as the infant grows.
The trachea’s greatest rate of growth occurs between 1 month and 4 years of age. The major growth of the airways is during the 10th to 14th week of gestation when 705 of the bronchial tree is established.
However, there are 2-4 generations of airways and large numbers of branches of these airways that will develop between the 24th week of gestation and term.
The surface area of the lung rapidly increases during the last trimester of pregnancy and during infancy. The term infant’s lung has approximately 55 million alveoli. This number will increase rapidly until the child’s lung has approximately 300 million alveoli at about 2 years of age.
The newborn infant has the potential for several intracardiac and extracardiac shunts. First, the ductus arteriosus is patent for the first 2-3 days of life. After birth, normally it will close in response to the increased blood PO2.
The foramen ovale is an opening in the interatrial septum that opens to allow blood to flow into the left atrium. It is functionally closed by the left atrial pressure being greater than the right atrial pressure.
Finally, the infant frequently has intrapulmonary shunts.
During intrauterine life, the infant shuts blood away from the lungs through the patent ductus arteriosus and the foramen ovale. The shunting occurs because of the pulmonary vascular resistance. After closure, any stimulus that causes a rise in the pulmonary vascular resistance has the potential to again cause a right to left shunt through either the foramen ovale or the ductus arteriosus.
The very compliant chest wall of the newborn allows for the necessary compression needed to permit the infant to pass from the uterus through the vaginal canal at birth.
Additionally, the lung of the infant is less compliant than the adult.
Higher chest wall compliance, lower lung compliance, and lower functional residual capacity are manifested by the infant as rapid shallow breathing.
The infant’s diaphragm is the major source of power for gas movement into the lung.
In the adult, during inspiration, the thoracic cavity increases longitudinally from top to bottom as well as circumferentially. Whereas, the infant’s thoracic cavity increases much more longitudinally in the top to bottom direction than it does circumferentially. Because there is less support of the chest wall by the accessory muscles, the greater expansion of the infant’s lung occurs at the bases.
Gas Transport
The presence of hemoglobin F changes the infant’s ability to transport oxygen from the lung to the tissues. Infant’s red blood cells with hemoglobin F will attach to oxygen more readily and will release oxygen less readily than the cells with hemoglobin A.
