Last Updated on October 29, 2023
Warts are a skin growth caused by viral infection. Warts are thought to occur when there is an infection of the skin by the papilloma virus. Papilloma virus is a DNA virus and is known to have more than 40 subtypes distinguished on the basis of the viral genome. Different subtypes are associated with different types of warts.
The virus grows only on the human skin and thus, the only source of infection is other infected individuals.
Warts are commonly seen in children, while adults generally develop immunity against this virus.
The infectivity of this virus is very low and therefore, a casual contact with an individual having these lesions is unlikely to result in infection.
Warts – How Does Virus Gain Entry Into Skin?
The virus enters the skin through microscopic abrasions and remains limited to the epidermis. The incubation period is variable and autoinoculation is frequent.
Clinical Presentation
Clinically, the lesions manifest in a variety of forms, but all types of lesions are asymptomatic, have an irregular verrucous surface and keep on growing at a very slow rate. A patient may have any number of lesions varying from one or two to a few hundred. Individuals with depression of the cell-mediated immunity due to lymphomas, AIDS or treatment with immunosuppressive drugs are more likely to have a large number of warts.
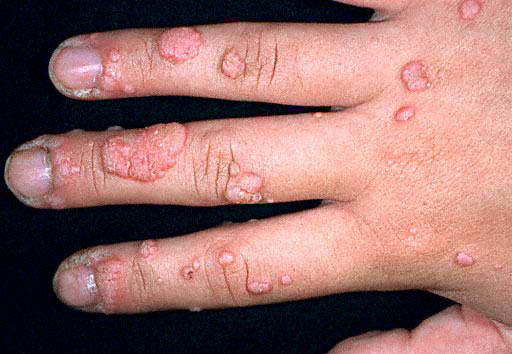
Verruca vulgaris
This is the most common variety and is caused by the viral types 1,2,4 and 7. The lesions consist of skin colored or brownish papules with an irregular surface which are usually present on the dorsal aspects of the hands, the forearms, and the face.
Rarely, the lesions may be present on the mucous membranes.
When lesions are present on the paronychial folds, or under the nail plate, these can be painful and also very difficult to treat.
Verruca plana
These are skin colored, flat-topped papules which are only slightly raised from the surface. These are usually seen on the dorsal aspects of the hands and the face. Plain warts are caused by the viral types 3, 10 and 28.
Filiform warts
These are finger-like projection of warty tissue usually present on the neck or the face.
Plantar warts
These are much bigger lesions caused by the virus types 1,2,4 and 7, which may occur in clusters on any part of the soles of the feet.
These lesions grow inside the skin and some of these lesions may also be painful.
Genital warts
These warts are also called condylomata acuminata. Most of these are caused by the subtypes 6 and 11 which have very low potential for malignancy, while a few of these caused by subtypes 16 and 30 have a high potential for malignant transformation.
Clinically, the lesions caused by any of these virus types are indistinguishable, and consist of fungating masses of verrucous tissue present on the anogenital region especially the glans in the male, and vulva, vagina, and cervix in the female.
These warts may also be seen in the perianal area, oral cavity or conjunctiva. These lesions grow much faster especially during pregnancy and are usually transmitted through sexual contact, and are thus far more common in the adults.
Treatment of Warts
None of the anti-viral drugs available so far are effective against warts. Thus, the only method of treatment consists of cauterization of the infected tissue with chemicals, electric heat, cryosurgery or laser therapy.
Chemical cauterization is usually done with liquefied phenol or concentrated trichloroacetic acid, but any other liquid capable of burning the skin can also be employed.
Immediately after cauterization, the tissue turns white and within two to three days, it turns brown or black. Within a week after cauterization, the whole crust falls off, leaving behind no mark of the original lesion.
For cauterization with electric heat, the electrically heated electrode should be applied on the surface of the lesion. The contact should be brief but repeated at different regions till the desired amount of tissue has been destroyed. Following this procedure as well, the lesion takes nearly one week for complete healing.
When the lesion is big, one should make a small incision with a scalpel all around the base of the wart and then scoop out the whole lesion with a metallic scoop. The wart, as a rule, comes out en mass, but this procedure should always be followed by cauterization of the base and the edges of the wound to destroy any infected tissue which may have been left behind. When electric cauterization is used, this procedure also ensures hemostasis.
Recurrence
Warts may reappear at the same site if they have not been completely destroyed or they may develop at new sites if the infection had already been transmitted to those sites. This is particularly common when the warts are present in the beard region where shaving promotes transplantation of the virus to the adjoining regions.
It is essential to destroy all the lesions.
Then, the patient should be examined again within a fortnight after treatment to ensure that there is no regrowth of the lesion and also to detect if there are new lesions.
Genital warts can be more easily treated with the local application of a 25 percent suspension of podophyllum in tincture benzoin. It is preferable to first apply vaseline on the skin surrounding the lesion to protect it from an overflow of the medicine. The podophyllum suspension should be allowed to dry and after two hours the whole area should be washed with soap and water.
Within a week’s time the wart may regress completely but in case the lesion is big, applications of podophyllum may have to be repeated at weekly intervals till the lesion regresses completely.
Podophyllum is effective only on genital warts and not on other types of lesions.
Many times, warts disappear even without any treatment.
