Last Updated on October 12, 2019
Epidermolysis Bullosa is a group of genetically inherited diseases in which the patient shows an enhanced tendency to develop blisters on areas subjected to minor trauma.
These diseases are also called mechano-bullous diseases.
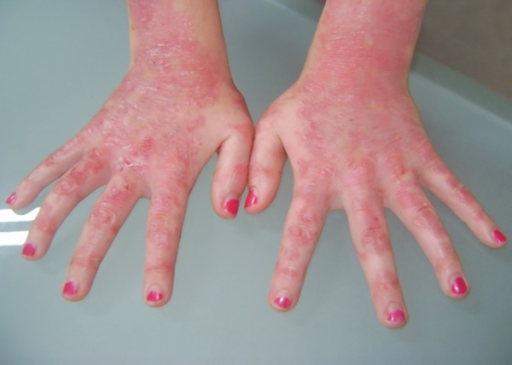
The blisters are usually situated on pressure points such as the toes, fingers, ankles, knees, wrists, and elbows and occasionally on the face as well. Areas of the body having a bone underlying the skin are the most frequently involved sites.
These blisters tend to heal rapidly unless they are subjected to repeated trauma or if they develop secondary infection. Some patients show ulceration of the mucous membranes and defective development of the nails.
There are at least 14 types of epidermolysis bullosa classified into 3 groups on the basis of clinical features, mode of inheritance and level of split formation in the skin.
The incidence of epidermolysis bullosa is 9.6- 54 cases per million live births in different countries.
The symptoms occur at birth or shortly after in all types except epidermolysis bullosa simplex, which could be asymptomatic and undetected until adulthood.
Pathophysiology
[Read anatomy of skin]
The disease is caused by an absence of basement membrane components that occur due to underlying gene mutations. Following categories of diseases are known
- Simplex (intraepidermal skin separation)
- Junctional (skin separation in lamina lucida or central basement membrane zone
- Dermal or dystrophic (sublamina densa basement zone separation)
- Kindler syndrome
Types of Epidermolysis Bullosa
Epidermolytic forms
Inherited as an autosomal dominant trait. They are characterized by the formation of splits in the epidermis by the degeneration of prickle or basal cells. These include:
Recurrent epidermolysis bullosa
- This occurs in hands and feet.
- The disease starts during late childhood or adult life.
- The blisters are limited to the palms and soles only.
- There is worsening in summer.
Epidermolysis bullosa simplex
- This can start soon after birth.
- Blisters occur on traumatized sites throughout the body.
- Mucosal and nail changes are minimal.
- Healing occurs without scars.
Epidermolysis bullosa simplex herpetiformis
- Blisters appear early and are generalized.
- The lesions tend to occur in herpetiform pattern.
- There is spontaneous recovery during fevers.
Epidermolysis bullosa simplex
- It is associated with small hypo and hyperpigmented macules.
- Later in life, the skin becomes atrophic and gets easily bruised.
- Palmo-plantar keratoderma may be associated.
- It occurs predominantly on the distal parts of extremities.
- It is associated with easy bruisability and worsening in summer.
Junctional forms
These are characterized by the formation of splits through the lamina lucida layer of skin deficient in hemidesmosomes. It has an autosomal recessive inheritance and a tendency to heal without scarring or milia formation. This group includes:
Epidermolysis bullosa atrophicans gravis
- It is almost uniformly fatal.
- It is characterized by severe blistering all over the body including the oral, gastrointestinal, respiratory, urogenital and conjunctival mucosae.
- The nails may be lost and the teeth may be dysplastic.
Epidermolysis bullosa atrophicans mitis
- It shows the involvement of skin, oral mucosa and, nails without the involvement of other organ systems.
- Improvement occurs as the child grows older.
Epidermolysis bullosa atrophicans inversa
- In this type, the blistering gets localized to the proximal parts of the extremities and the intertriginous areas of the perineum, axillae and neck.
- The traditional pressure sites are spared.
Epidermolysis bullosa atrophicans localisata
- The lesions are localized to the lower extremities and soles.
- Aggravations occur in summer.
- Onset occurs at school-going age.
Epidermolysis bullosa progressiva
- As the name suggests, the severity increases with age.
- Age of onset is 5 years
- Nail changes occur before the skin lesion.
Dermolytic form
This includes the types in which the blistering occurs below the basement membrane due to defective anchoring fibrils or by their dissolution due to an excess of collagenase. They occur both in autosomal dominant and recessive forms. These types are associated with severe scarring and milia formation.
Recessive epidermolysis bullosa dystrophica
- There is severe blistering and scarring all over the skin, oral mucosa, conjunctiva and cornea, esophagus, trachea, urethra with strictures.
- Loss of nails.
- Cicatricial alopecia (Baldness).
- Loss of teeth.
Recessive epidermolysis bullosa dystrophica inverse
- The lesions are localized to intertriginous areas such as groins, axillae, neck, trunk, and perianal area. An intertriginous area is an area where opposing skin surfaces touch and may rub, such as skin folds of the groin, axilla, and breasts.
Dominant epidermolysis bullosa dystrophica
- It involves the skin on the traumatized sites.
- Scarring and milia formation.
- Oral mucosa, nails, cornea and conjunctiva are involved.
Dominant epidermolysis bullosa dystrophica Albopapuloid
- Skin colored or whitish papules appear on the trunk at about puberty in addition to the blisters, scarring and milia which occur since birth.
Other varieties are quite rare.
Clinical Presentation
There would be a history of multiple blisters which begins in early life. Size, frequency, and location of blisters is enquired along with family history. All the skin and mucosal surfaces such as conjunctival, oral, and genital should be examined for blisters.
Differential Diagnoses
- Bullous disorders
- Friction Blisters
- Burns
- Insect Bites
- Pemphigus Vulgaris
Diagnostic Work-up
Routine microscopic analysis can be used to rule out other causes of blisters but are not able to diagnose epidermolysis bullosa.
For diagnosis two specimens are taken for electron microscopy and immunofluorescent microscopy.
Electron microscopy determines the level of blistering epidermal, junctional or dermal.
Immunofluorescent microscopy can reveal the level of blistering as well as provide an important clue regarding the underlying molecular defect.
However, DNA mutation test is better at showing the underlying molecular defect
DNA analysis can also help in prenatal diagnosis.
Other evaluations are as follows
- Anemia in severe disease
- CBC
- Iron Studies
- Infection
- Culture from discharge or poorly healing wounds
- Gastrointestinal dysfunction
- Esophageal strictures in junctional/dystrophic types
- Pyloric atresia
- Nutrition
- Serum albumin
- Height and weight curves
Treatment
The mainstay of treatment in all these cases is to protect the individual from trauma.
Care has to be taken to protect the patient even from those minor trauma that occur during one’s daily activities and which as a rule, go unnoticed, but the intensity of these measures will depend upon the severity of the disease.
During infancy, the patient has to be handled very gently.
The clothes have to be soft, padded and loose and should not produce friction at any site. As the child grows, he should avoid activities likely to expose him to trauma. The blisters may be punctured but the roof of the blister must not be removed.
The dressings or the clothes should not be allowed to stick to the skin lesions and should be removed very gently.
Adhesive tapes should never be applied to the skin.
Treatment of Acute Blisters
- Aggressive treatment of wound by proper wound care
- Infections should be prevented and when occur treated with antibiotics
- Vitamin E in a dose of 100 mg once or twice a day has been used in the epidermolytic type of epidermolysis bullosa simplex.
- Phenytoin 2-4 mg per kg body weight a day has been used for the dermolytic types with good results.
These drugs bring about only a decrease in the severity of the disease.
Long Term Treatment
Systemic corticosteroids may also be used for short periods to tide over difficult phases of the disease. These are also used for esophageal strictures.
Patients should be monitored for squamous cell carcinoma and treated accordingly.
Corneal erosions
- Antibiotic ointment
- Cycloplegic agents to reduce ciliary spasm.
Cicatricial ectropion and exposure keratitis
- Moisture chambers
- Ocular lubricants are used commonly for management
- Full-thickness skin grafting to the upper eyelid.
Esophageal strictures can surgically be managed by esophageal dilation.
Surgical restoration of the hand for Mitten deformity.
Surgical excision of squamous cell carcinoma
Prognosis
Epidermolysis bullosa stays for life though some milder varieties show improvement with age.
Infection, sepsis, and death may complicate the blistering, especially in infancy. Other complications are
- Squamous cell carcinoma
- Pseudosyndactyly (mitten-hand deformity)
- Skin grows around the digit and encases them over a period
- Esophageal scarring secondary to repeated blistering and healing
- Oral inflammation
Severe forms of the disease have a very high mortality rate.
The most common cause of death in survivors is metastatic squamous cell carcinoma.
References
- Sawamura D, Nakano H, Matsuzaki Y. Overview of epidermolysis bullosa. J Dermatol. 2010 Mar. 37(3):214-9
- Fine JD, Bauer EA, McGuire J, Moshell A, eds. Epidermolysis Bullosa: Clinical, Epidemiologic, and Laboratory Advances and the Findings of the National Epidermolysis Bullosa Registry. Baltimore, Md: Johns Hopkins University Press; 1999.
- Tong L, Hodgkins PR, Denyer J, et al. The eye in epidermolysis bullosa. Br J Ophthalmol. 1999 Mar. 83(3):323-6.
- McAllister JC, Peter Marinkovich M. Advances in inherited epidermolysis bullosa. Adv Dermatol. 2005. 21:303-34.
