Last Updated on October 29, 2023
Ascites refers to the collection within the abdominal cavity. In Greek, the word askos means bag or sac.
The collected fluid is called the ascitic fluid.
It can be caused by many disorders but the most common cause is portal hypertension due to cirrhosis which results in increased pressure in the veins that bring blood to the liver.
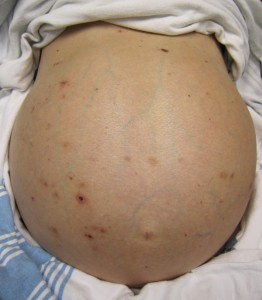
Mild condition may not be noted but when a large amount of fluid accumulates, it could cause visible fullness of abdomen and other symptoms.
By definition, the presence of greater than 25ml of fluid is considered as ascites.
It must be noted that healthy men have little or no intraperitoneal fluid. Women, depending on the menstrual cycle phase, can have up to 20 mL.
It is a symptom of another underlying cause rather than being a disease itself. Therefore, the treatment of ascites is directed at the treatment of the underlying cause.
Causes of Ascites
As much as 75% of cases of ascites are due to portal hypertension following cirrhosis of the liver. Ascites tends to occur after the liver disease of long duration.
Before we look into causes, we must understand SAAG or serum ascites albumin gradient. It is a value calculated to determine the probable causes as peritoneal or nonperitoneal.
The formula is
SAAG = serum albumin – ascitic fluid albumin
A high gradient (SAAG >1.1 g/dL) suggests that the cause is portal hypertension which could be caused by liver or non-liver causes.
The ascitic fluid is transudative.
A low gradient (SAAG < 1.1 g/dL) indicates nonportal hypertension and suggests a peritoneal cause and the ascitic fluid is exudative.
SAAG>1.1 g/dL
That indicates that peritoneum is normal. The causes are outside the peritoneum
- Cirrhosis
- Alcoholic liver disease
- Viral hepatitis
- Cryptogenic
- Massive liver metastases
- Fulminant hepatic failure
- Hepatic congestion due to right-sided heart failure
- Congestive heart failure
- Constrictive pericarditis
- Tricuspid insufficiency
- Budd-Chiari syndrome
- Hypoalbuminemia
- Nephrotic syndrome
- Protein-losing enteropathy
- Severe malnutrition
SAAG <1.1 g/dL
With SAAG less than 1.1 the cause is often peritoneal involvement.
- Infections
- Bacterial peritonitis
- Tuberculous peritonitis
- Fungal peritonitis
- Human immunodeficiency virus (HIV)-associated peritonitis
- Malignant conditions
- Peritoneal carcinomatosis/metastasis
- Primary mesothelioma
- Pseudomyxoma peritonei
- Hepatocellular carcinoma
- Miscellaneous conditions
- Chylous ascites – Chyle or lymph extravasation
- Pancreatic ascites [pancreatitis]
- Bile ascites
- Nephrogenic ascites
- Urine ascites
- Ovarian disease
- Familial Mediterranean fever
- Vasculitis
- Granulomatous peritonitis
- Meigs syndrome
- Hereditary angioedema
Pathophysiology
The exact mechanism is not clear Following theories have been propagated.
Underfilling Theory
- Primary abnormality is an inappropriate collection of fluid within the visceral region due to portal hypertension
- It results in a decrease in effective circulating blood volume.
- Water conservation system [plasma renin, aldosterone, and sympathetic nervous system] gets activated causing sodium and water retention.
Overflow theory
It maintains that primary abnormality is inappropriate sodium and water retention by kidney though there is no reduction of circulatory volume.
[It has been noted that that patient with cirrhosis has intravascular hypervolemia rather than hypovolemia.]
Peripheral Arterial Vasodilation
This theory suggests that portal hypertension leads to vasodilation which causes decreased effective arterial blood volume. [There are increased nitric acid levels which cause vasodilation. Hepatic artery nitric oxide synthase activity is greater in patients with ascites.
With disease progression, under the influence of neural and hormonal factors, kidney works to retain sodium and expansion of plasm volume occurs.
This causes an overflow of fluid into the peritoneal cavity.
Other factors that contribute to ascites
- Increased levels of epinephrine and norepinephrine
- The decrease in blood albumin levels (Hypoalbuminemia) decreases plasma oncotic pressure. This favors fluid extravasation from plasma to the peritoneal fluid.
Patients at Risk
As the liver disease is the most common cause, the risk factors for liver disease are the risk factors of ascites also.
- Chronic alcohol use
- Intravenous drug user
- Drug abuse
- History of viral hepatitis
- Multiple sexual partners
- Multiple transfusions
- Hepatocellular carcinoma
- Risk factors for NASH (nonalcoholic steatohepatitis)
- Obesity
- Increased levels of cholesterol
- Type 2 diabetes mellitus
- History of gastrointestinal cancer
Symptoms and Signs [Clinical Presentation]
Small amounts of fluid within the abdomen usually cause no symptoms. Moderate amounts may increase a person’s waist size and cause weight gain. Massive amounts may cause abdominal swelling (distention) and discomfort. The abdomen feels taut, and the navel is flat or even pushed out.
The swollen abdomen puts pressure on the stomach, sometimes leading to loss of appetite and pressure on the lungs, sometimes leading to shortness of breath.
In some people with ascites, the ankles swell because excess fluid accumulates there (causing edema).
On examination, in liver disease, jaundice may be noted. Palmar erythema and spider angiomas are other signs of liver disease.
The liver may be enlarged but difficult to palpate because of ascites.
Depending on the causation other signs and symptoms may be present. A raised jugular venous pressure suggests a cardiac problem.
Lab Studies
Routine blood work should be done. The mainstay of the diagnosis is a study of ascitic fluid which is removed by a procedure called paracentesis.
The ascitic fluid is studied for biochemistry, cytology, and microbiology.
Normal peritoneal fluid is yellowish and transparent. A pink or red indicates the presence of red blood cells.
Cloudy or purulent fluid suggests infection.
WBC count is normally less than 500 leukocytes per microliter and less than 250 neutrophils (polymorphonuclear cells).
A higher neutrophil count suggests bacterial peritonitis.
SAAG is calculated as per the previously described formula.
High SAAG with high total level is suggestive of hepatic congestion whereas low SAAG with high protein indicates malignant ascites.
Cultures are used to identify bacteria in suspected infection or to find if pancreatitis is present [ascitic amylase cultures]
Cytological studies can help to detect malignant ascites.
Imaging
X-rays
X-ray chest and abdomen, though commonly done, require a fluid buildup of about 500 ml before they could suggest. Thus x-rays are not the sensitive investigation.
When ascites is present x-rays may reveal the following
- Medial displacement of lateral liver edge (Hellmer sign)
- Mickey Mouse or Dog Ear Sign
- Symmetric densities on both sides of the bladder
- Due to fluid in rectovesical pouch and the paravesical fossa.
- Medial displacement of the cecum and ascending colon
- Lateral displacement of the preperitoneal fat
- Non-specific signs
- Elevation of the diaphragm [in massive ascites.]
- Non-specific signs
- Diffuse haziness of abdomen
- Bulging of the flanks
- Separation of small bowel loops
- Centralization of floating gas containing small bowel
- Unclear psoas margin
Ultrasound
It is a very sensitive method of fluid detection and can identify as low as 5-10 mL.
Ultrasound can help to identify infection, inflammation or malignancy.
CT
CT can also identify a small amount of fluid which is often localized in the right perihepatic space, the posterior subhepatic space, and the Douglas pouch
CT scan is able to suggest if the cause is malignant.
Diagnostic Laparoscopy
For unexplained cases, especially if malignant ascites is suspected.
Treatment
Medical treatment of ascites involves the following
- A low-sodium diet and bed rest
- Diuretics – class of drugs that increase the flow of urine
- Therapeutic paracentesis – drainage of ascitic fluid to reduce the load
- Surgery to reroute blood flow or liver transplantation
- Treatment of underlying cause or complications
The basic treatment for ascites is a low-sodium diet.
Sodium restriction and diuretic therapy are standard medical management.
Therapeutic paracentesis [removal of fluid by inserting the needle in paritoneum] may be performed for
- Faster relief
- For palliative care as in malignant ascites
Albumin may be given intravenously to replenish lost albumin from blood to ascitic fluid.
Transjugular intrahepatic portosystemic shunt (TIPS) is a shunt procedure.
A shunt is an artificial passage which allows fluid to move from one part of your body to another.
TIPS connects portal vein which brings the blood from gastrointestinal tract and intra-abdominal organs to hepatic vein by a stent which creates a bypass and reduced load on the liver.
TIPS is gradually becoming the standard of care in patients with diuretic-refractory ascites.
The peritoneovenous shunt is an alternative.
Spontaneous bacterial peritonitis is a common complication which requires treatment by antibiotics.
The patient is regularly monitored by measuring body weight and urinary sodium levels.
The treatment is adjusted according to the response of the patient.
Prognosis of Ascites
Patients who are ambulatory and have an episode of cirrhotic ascites have 50% mortality rate at 3 years. That means only 50% survive after 3 years.
A refractory ascites carries even a poor prognosis, with a 1-year survival rate of less than 50%.
The prognosis depends on the underlying disorder and the response to treatment.
Complications
- Spontaneous bacterial peritonitis [most common]
- Electrolyte disturbance
- Bleeding
- Bowel perforation
- Kidney injury
References
- Pericleous M, Sarnowski A, Moore A, Fijten R, Zaman M. The clinical management of abdominal ascites, spontaneous bacterial peritonitis and hepatorenal syndrome: a review of current guidelines and recommendations. Eur J Gastroenterol Hepatol. 2016 Mar. 28(3):e10-8.
- Peritoneal catheter for continuous drainage of ascites in advanced cancer patients. Support Care Cancer. 2008 Aug. 16(8):975-8.
.
